Understanding Hip Bursitis: Symptoms, Causes, and Effective Treatments
Your complete guide to hip bursitis, including symptoms, causes, prevention, and the latest effective natural treatment options.
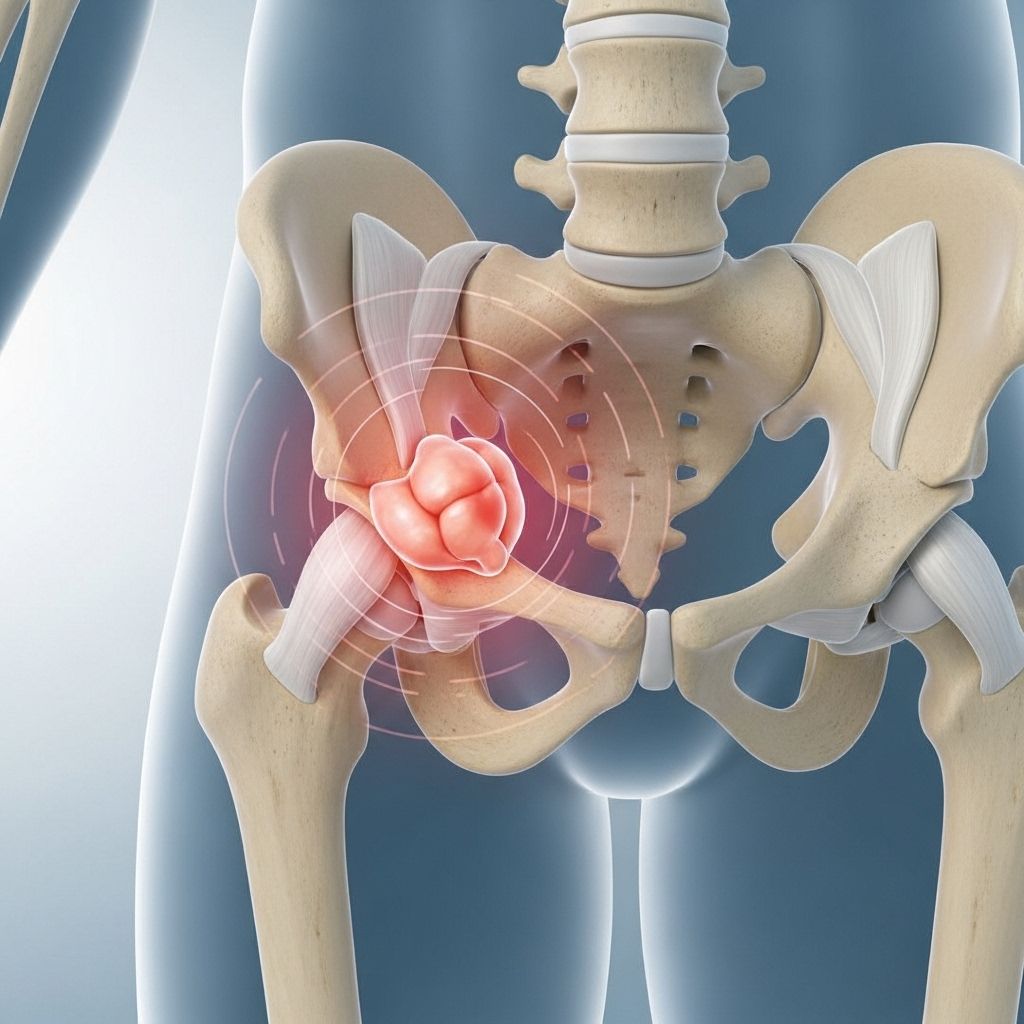
Hip Bursitis: A Comprehensive Guide
Hip bursitis is a common and often painful condition, characterized by inflammation of the bursa—a small, fluid-filled sac that cushions and eases movement in your hip joint. The following guide explains everything you need to know about hip bursitis, from symptoms and causes to proven prevention methods and the latest in natural and conventional treatments.
What Is Hip Bursitis?
The hip contains multiple bursae, but inflammation most often occurs in the trochanteric bursa located on the outer side of the hip. The bursa acts as a cushion, helping reduce friction as muscles and tendons glide over bones. When these sacs become irritated, often due to repetitive movements or pressure, the result is hip bursitis—one of the leading causes of hip pain in adults.
Understanding the Bursa and Its Role in the Hip
Bursae are present throughout the body, particularly near major joints like the hip, knee, and shoulder. In the hip, the most notable bursae include:
- Trochanteric bursa: Found on the outside of the hip, most frequently affected by bursitis.
- Iliopsoas bursa: Located on the inside of the hip, can lead to groin pain when inflamed.
- Ischial bursa: Found near the buttocks, less commonly affected.
Healthy bursae allow painless gliding during hip movement. When inflamed, these structures lose their cushioning capacity, causing pain and restricted motion.
Symptoms of Hip Bursitis
The most common symptoms of hip bursitis can significantly impact daily activities. Watch for the following signs:
- Pain on the outside of the hip, often radiating down the thigh.
- Tenderness when pressing over the outer hip area.
- Swelling and a feeling of heat or warmth near the affected bursa.
- Sharp, intense pain initially that may become dull and achy over time.
- Stiffness or difficulty while walking, climbing stairs, or rising from a chair.
- Pain that worsens after prolonged standing, moving, or sleeping on the affected side.
- Possible redness if the bursa is infected (septic bursitis).
For some, hip bursitis may develop suddenly following injury, but symptoms often arise gradually and worsen with ongoing activity.
Causes and Risk Factors: Why Does Hip Bursitis Occur?
Bursitis occurs when one or more bursae in the hip become irritated, producing excess fluid and swelling. The main causes include:
- Overuse and repetitive stress from sports, manual labor, or repeated movements.
- Direct injury such as a fall, bump, or impact to the hip.
- Underlying conditions like rheumatoid arthritis, gout, or diabetes.
- Bacterial infection (septic bursitis), though less common.
- Structural issues, such as scoliosis, leg-length differences, or presence of bone spurs.
- Other hip problems (e.g., torn tendons, spine problems) increasing friction over the bursa.
| Risk Factor | Details |
|---|---|
| Age | Incidence increases with advancing age. |
| Occupation/Hobby | Jobs or sports involving repetitive hip motion (e.g., running, carpentry, gardening). |
| Obesity | Excess weight increases pressure and friction on hip bursae. |
| Medical Conditions | Inflammatory diseases, metabolic disorders, spine issues. |
Types of Hip Bursitis
- Trochanteric bursitis: Most common, causing pain on the outer hip.
- Iliopsoas bursitis: Causes pain in the groin or inner hip.
- Septic bursitis: Bacterial infection of the bursa, often with fever and redness.
How Is Hip Bursitis Diagnosed?
Diagnosing hip bursitis typically involves a physical examination and a review of your symptoms and medical history. In some cases, additional tests may be needed to rule out other conditions or confirm the diagnosis:
- Physical examination: Palpation over the hip, assessment of pain and mobility.
- Imaging tests: X-rays to rule out arthritis or bone problems; MRI to visualize soft tissues.
- Fluid analysis: In cases of suspected infection, a sample of fluid from the bursa may be tested for bacteria.
Can Hip Bursitis Be Prevented?
While not all cases of hip bursitis can be avoided, certain strategies can significantly reduce your risk or limit recurrence:
- Avoid repetitive hip movements whenever possible, or take frequent breaks.
- Use proper technique when lifting or performing sports to minimize joint stress.
- Warm up and perform stretching exercises before activity.
- Strengthen hip and core muscles to better support and stabilize the joint.
- Maintain healthy body weight to reduce excess pressure on the hips.
- Address leg-length differences with lifts or orthotics if prescribed.
Conventional Treatments for Hip Bursitis
The majority of hip bursitis cases resolve without the need for surgery, especially with early and consistent non-invasive care:
- Rest and Activity Modification: Limit activities that increase pain, such as long walks or stairs.
- Ice Therapy: Apply cold packs to reduce swelling and pain, especially within the first 72 hours.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter medications such as ibuprofen and naproxen help control inflammation and pain (always consult your doctor before prolonged use).
- Physical Therapy: Targeted exercises and stretches can improve hip flexibility, strength, and correct posture abnormalities. Physical therapists may also employ massage, ultrasound, or rolling therapy to address tightness and promote healing.
- Assistive Devices: Temporary use of a cane, crutches, or orthotics can reduce joint stress during recovery.
- Corticosteroid Injections: If pain persists, a doctor may recommend injecting a steroid directly into the bursa to decrease inflammation. This can provide relief for several months but should be limited due to potential tissue damage with repeated use.
- Antibiotics for Septic Bursitis: If infection is present, antibiotics are essential, and hospitalization may be needed for severe cases.
Surgical Treatment
Surgery is rarely required for hip bursitis. When all other options fail and pain is persistent and disabling, surgical removal of the bursa may be considered. Today, minimally invasive techniques such as endoscopic or arthroscopic removal allow for faster recovery and less risk. Importantly, removal of the bursa does not impair hip function long-term.
Natural Alternatives and Home Management Strategies
Many people seek ways to manage or prevent hip bursitis naturally. Adjunctive measures and lifestyle adaptations can further enhance recovery and reduce reliance on medication:
- Apply a natural osmosis patch or similar products to reduce swelling by drawing out excess fluid from the affected area.
- Gentle stretching routines focusing on the iliotibial (IT) band, gluteal muscles, and hip flexors.
- Weight management through a balanced diet and regular, low-impact exercise.
- Anti-inflammatory diet emphasizing Omega-3-rich foods, leafy greens, and turmeric.
- Massage therapy to address tight muscles and fascia in the hip region.
- Acupuncture for pain and inflammation moderation (when performed by a qualified provider).
- Heat application after the acute phase to relax tight muscles around the hip.
Living with and Preventing Recurrence of Hip Bursitis
After initial recovery, lifestyle modifications and regular exercise are the best path forward:
- Incorporate strength and flexibility routines targeting the hip, gluteal, and core muscles.
- Avoid any activity that triggers a flare-up or repeat irritation.
- Use proper alignment and ergonomic aids if your work or daily activities demand repetitive hip motion.
- Maintain a healthy weight to continue minimizing pressure on the joint.
Education, prevention, and proactive management are key to sustained hip health.
Frequently Asked Questions (FAQs) about Hip Bursitis
Q: What is the main symptom of hip bursitis?
A: The most common symptom is pain and tenderness over the outer side of the hip, worsening with movement or pressure, such as when lying on the affected side.
Q: How can I tell hip bursitis from arthritis or other hip pain?
A: Bursitis pain usually stays localized to the outer hip and may radiate down the thigh, whereas arthritis pain is typically more diffuse or deep in the groin. Your healthcare provider may order tests to confirm the diagnosis.
Q: How long does it take for hip bursitis to heal?
A: With prompt treatment and activity modification, many cases resolve within a few weeks, although chronic or severe cases may take several months for complete recovery.
Q: Can I exercise with hip bursitis?
A: Light exercises and physical therapy are encouraged, but high-impact activities or anything that worsens your symptoms should be avoided until pain subsides.
Q: When should I see a doctor?
A: If you experience fever, redness, intense pain, or if your symptoms do not improve with self-care after two weeks, consult a healthcare professional. Seek urgent care for signs of infection or loss of hip function.
Q: Are natural therapies effective for hip bursitis?
A: Many people experience relief from adjunctive natural methods like stretching, osmosis patches, dietary changes, and gentle massage, especially when combined with conventional treatment.
Key Takeaways for Managing Hip Bursitis
- Hip bursitis is common, often responsive to rest, lifestyle adaptation, and natural support measures.
- Pay attention to symptoms and reduce activities that aggravate the joint.
- Strength, flexibility, and a healthy weight reduce the risk of flare-ups.
- Consult a healthcare provider for proper diagnosis, especially if pain is intense or persistent.
- Integrate both medical and natural therapies for comprehensive, sustained hip pain relief.
Read full bio of medha deb











