Aortic Valve Calcification: Early Indicator and Management of Heart Valve Disease
Understanding aortic valve calcification as an early sign of heart disease risk, clinical implications, and treatment options for better heart health.
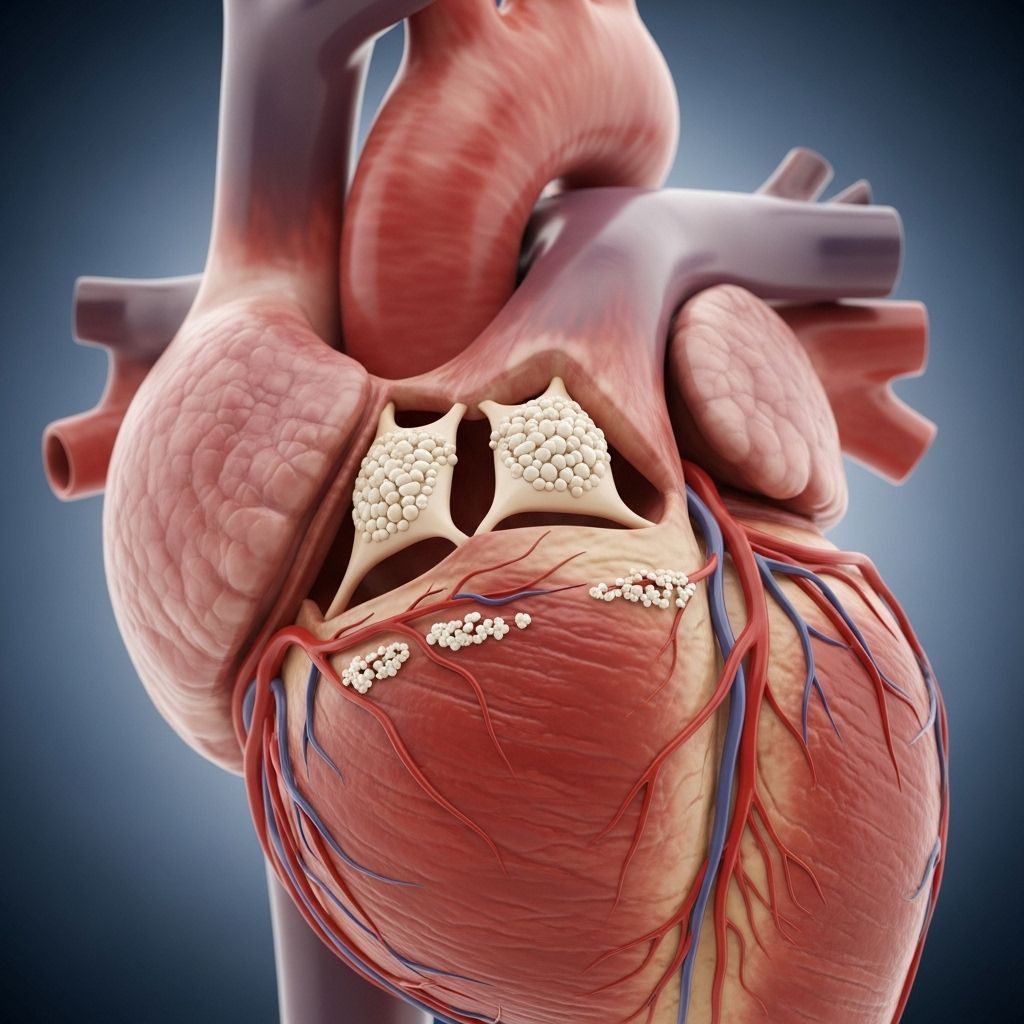
Aortic Valve Calcification: An Early Sign of Heart Valve Problems?
Aortic valve calcification is increasingly recognized as a critical marker for emerging heart valve complications. Characterized by the buildup of calcium deposits on the aortic valve, this condition can signal a progressive narrowing (stenosis) of the valve opening, often before overt symptoms of heart disease manifest. Timely recognition and management of aortic valve calcification are vital for maintaining optimal cardiovascular health and preventing further complications.
What is the Aortic Valve?
The aortic valve separates the heart’s lower left chamber (left ventricle) from the aorta, the body’s principal artery. Its main function is to ensure one-way, uninterrupted blood flow from the heart into systemic circulation. Any form of obstruction or stiffening—such as that caused by calcification—can result in diminished cardiac output and strain on the heart muscle.
Is Aortic Valve Calcification a Sign That I Am Starting to Get Heart Disease?
Aortic valve calcification is a condition wherein calcium builds up on the aortic valve leaflets. This process causes the valve to become stiff, and the opening may narrow—a phenomenon termed aortic stenosis. Severe stenosis can critically reduce or block blood flow, making the heart work harder to pump blood throughout the body. Importantly, the presence of aortic valve calcification may indicate the onset of heart disease, even in the absence of other classical symptoms.
- Most commonly affects adults over 65 years.
- Early stages may be symptom-free.
- Progression can lead to significant symptoms and complications.
Causes of Aortic Valve Calcification
While aging is the most prominent factor in aortic valve calcification, younger individuals may develop the condition due to:
- Congenital heart defects, such as bicuspid aortic valve (in which only two valve leaflets are present instead of three).
- Chronic illnesses: For example, kidney failure or familial hypercholesterolemia (an inherited tendency toward high cholesterol).
- Chronic inflammation and oxidative stress that accelerate calcific processes.
Mild calcium buildup may also occur with aortic valve sclerosis, a condition marked by valve thickening and stiffness but often not severe enough to cause major heart problems. Nevertheless, sclerosis can gradually progress to stenosis requiring further medical intervention.
Who Is at Risk?
Certain factors make individuals more susceptible to developing aortic valve calcification:
- Advanced age (most common in people over 65).
- Congenital defects, e.g., bicuspid aortic valve.
- History of kidney disease or chronic renal failure.
- Longstanding high cholesterol (including genetic forms).
- Other risk factors: Hypertension, diabetes, smoking, and male sex have been linked to increased risk.
Symptoms and Signs of Aortic Valve Calcification and Stenosis
Aortic valve calcification does not immediately cause symptoms. When it progresses to significant stenosis, however, patients may experience:
- Shortness of breath or decreased exercise tolerance
- Chest pain (angina)
- Fainting or dizziness (syncope or presyncope)
- Fatigue
- Fluid retention (edema, often in lungs and ankles)
- Heart murmur (audible abnormal heart sound signifying turbulent blood flow)
Less commonly, advanced cases may cause heart failure symptoms, gastrointestinal bleeding (due to acquired von Willebrand factor deficiency), or cerebral emboli.
Progression of Symptoms
- Early stages: Mild or no symptoms; detected via routine exams or imaging.
- Moderate stenosis: Reduced physical capacity, exertional breathlessness.
- Severe stenosis: Prominent chest pain, marked shortness of breath, syncope, and risk of sudden cardiac death.
Diagnosis of Aortic Valve Calcification and Stenosis
The diagnosis involves a combination of clinical assessment, physical examination, and advanced imaging:
- Physical exam: May reveal a harsh, late-peaking systolic murmur (often radiating to the carotid arteries) and a slow carotid pulse. However, findings are often subtle, especially in older patients or those with coexisting vascular disease.
- Echocardiogram (ECHO): The gold standard; provides visualization of valve structure, leaflet motion, calcification extent, and measures valve area and transvalvular flow velocity.
- Other tests: Chest X-ray, ECG, and blood biomarkers may provide supportive information but are less specific.
| Test | Use | Key Findings |
|---|---|---|
| Physical Exam | Initial assessment | Murmur, pulse changes |
| Echocardiogram | Detection and quantification | Calcification, valve area, flow velocity |
| Chest X-ray | Assess heart size and valve | Heart enlargement, valve calcification |
| ECG | Check heart rhythm/function | LV hypertrophy, arrhythmias |
Complications of Aortic Valve Calcification
If left untreated, progressive calcification and resulting stenosis can lead to significant complications, including:
- Heart failure
- Arrhythmias (irregular heartbeats)
- Stroke or embolic events
- Sudden cardiac death (especially in severe cases)
- Infective endocarditis (risk increases with damaged valves)
Management and Treatment Options
Management depends on severity of calcification and degree of stenosis:
- Mild calcification (sclerosis): Regular monitoring and risk factor modification (control blood pressure, cholesterol, diabetes, and address lifestyle factors).
- Moderate to severe stenosis:
- Referral to a cardiologist for advanced management.
- Medical therapy to relieve symptoms (diuretics, ACE inhibitors, beta-blockers), though no medication reverses calcification.
- Valve replacement or repair for severe or symptomatic cases. Surgical options include minimally invasive transcatheter aortic valve replacement (TAVR) and open-heart valve surgery.
- Treatment of associated conditions (management of arrhythmias, infections, or anemia)
Prevention and Risk Reduction
- Control cholesterol and use statin therapy if indicated.
- Management of hypertension.
- Optimal diabetes control.
- Smoking cessation.
- Regular cardiac checkups, especially if heart murmurs or risk factors are present.
Living with Aortic Valve Calcification
Many individuals with early-stage calcification or sclerosis remain asymptomatic and can lead healthy lives with ongoing monitoring. For those progressing to clinical stenosis, lifestyle modifications and adherence to medical recommendations are essential for improving outcomes and preventing complications. Discussing treatment plans with a cardiologist and understanding when surgical intervention may become necessary is critical.
Frequently Asked Questions (FAQs)
- Q: Is aortic valve calcification reversible?
- A: No current medication or treatment can reverse established calcification. Management focuses on slowing progression, symptom relief, and timely intervention if stenosis develops.
- Q: Should I worry if I have aortic valve sclerosis?
- A: Mild thickening and stiffness (sclerosis) alone often do not cause major problems, but regular checkups are necessary to monitor for worsening or progression to stenosis.
- Q: What symptoms should prompt a doctor’s visit?
- A: Report new chest pain, shortness of breath, fainting, severe fatigue, and noticeable swelling, as these symptoms may indicate progression to significant stenosis.
- Q: What is the treatment for severe aortic valve stenosis?
- A: Severe cases often require valve replacement surgery or TAVR. No medicines can “cure” severe stenosis once symptoms appear; prompt evaluation and intervention are necessary.
- Q: Are younger people at risk?
- A: Yes, particularly those with congenital heart defects (e.g., bicuspid aortic valve) or chronic illnesses such as renal failure or inherited high cholesterol.
Key Takeaways
- Aortic valve calcification is an early indicator of potential heart valve disease, increasing in prevalence with age.
- Watch for symptoms such as chest pain, shortness of breath, fainting, and heart murmur. Early detection improves outcome.
- Echocardiography is critical for diagnosis and assessing severity.
- Management ranges from risk modification and monitoring to surgical intervention in advanced cases.
- Consult a cardiologist if any symptoms develop or imaging suggests valve abnormalities.
Resources for Patients and Families
- Regular follow-up with primary care and cardiology providers.
- Access educational material from major heart health organizations.
- Adopt healthy lifestyle habits and monitor cardiovascular risk factors.
Conclusion
Aortic valve calcification merits attention as part of routine cardiovascular health assessments. By recognizing risk factors, understanding the progression to aortic stenosis, and engaging in proactive management, individuals and healthcare providers can reduce the risk of serious heart complications and promote long-term wellness.
Read full bio of Sneha Tete