Bartter Syndrome: Causes, Symptoms, Genetics, and Management
A comprehensive guide to Bartter syndrome—exploring its genetic origins, key symptoms, subtypes, risk factors, diagnosis, and treatment options.
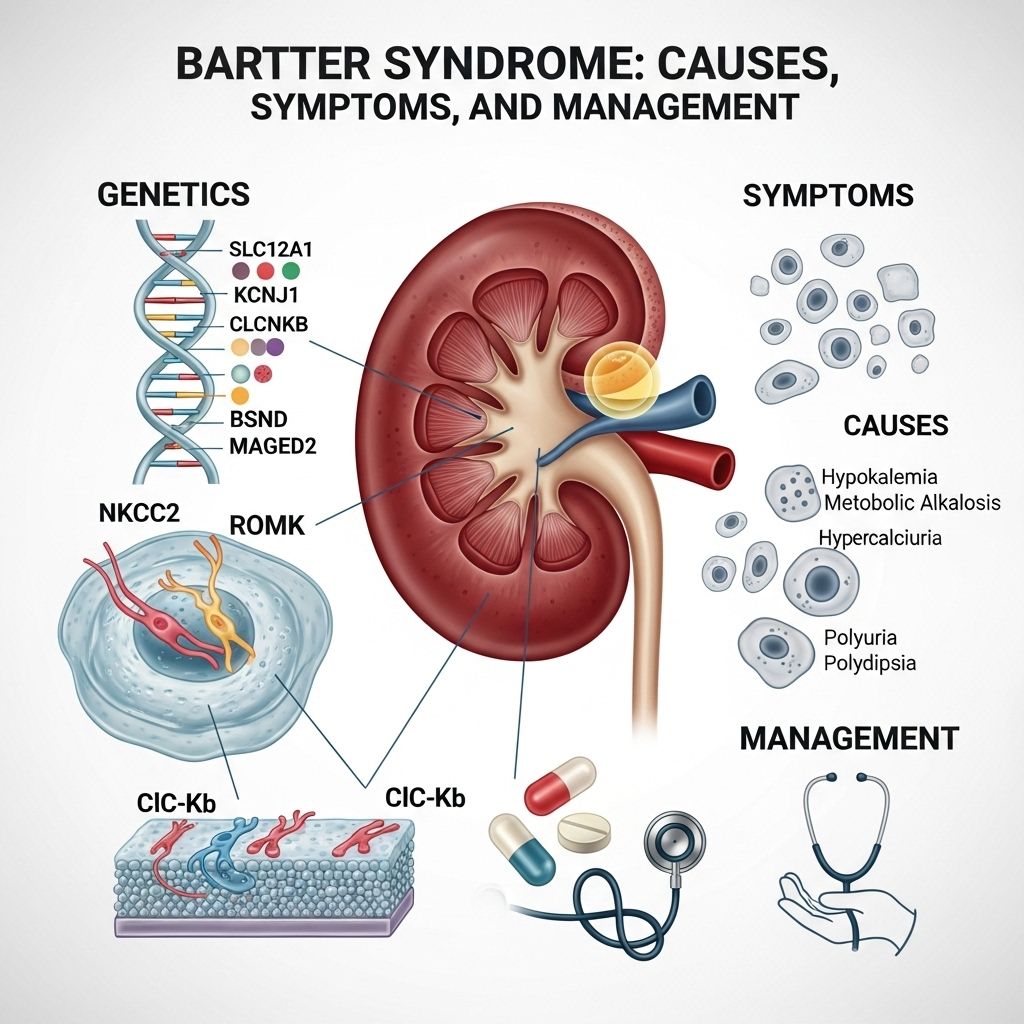
Bartter Syndrome
Bartter syndrome refers to a group of rare, genetically inherited kidney disorders that disrupt the body’s ability to balance certain salts and electrolytes, especially potassium, sodium, and chloride. This imbalance arises from abnormal functioning of the kidney tubules, leading to excessive loss of vital minerals in the urine. These disorders are collectively associated with various symptoms ranging from muscle weakness to growth problems, and are present from birth.
Overview
Bartter syndrome includes several closely related disorders characterized primarily by impaired reabsorption of sodium and chloride in the kidneys. The kidneys normally play a key role in maintaining the concentration of electrolytes in the body. In Bartter syndrome, gene mutations impair the ability of renal tubules—specifically parts of the nephron called the loop of Henle and, in some cases, the distal convoluted tubule—to reabsorb these crucial ions, resulting in their excessive renal loss and triggering a cascade of compensatory and pathological changes within the body.
The spectrum of Bartter syndrome is variable, with some forms being more severe than others, and symptoms may manifest before birth, in infancy, or during childhood.
- Disorder type: Congenital (present at birth), genetically inherited
- Main effect: Imbalance of potassium, sodium, chloride, and related molecules
Signs and Symptoms
The specific signs and symptoms of Bartter syndrome can differ depending on the subtype and severity, but common features include:
- Frequent urination (polyuria)
- Excessive thirst (polydipsia)
- Dehydration, often mild but persistent
- Growth delays or failure to thrive (especially in infants and children)
- Muscle weakness, cramps, and spasms
- Constipation
- Low blood pressure (hypotension)
- Abnormal heart rhythms (arrhythmias)
- Vomiting and nausea
- Salt craving
- Hearing loss (in certain subtypes)
Symptoms often develop in childhood, but some types of Bartter syndrome present in the pre-birth (antenatal) period. In these cases, excessive production of amniotic fluid (polyhydramnios) may be detected, and newborns may have severe salt and water imbalances at birth.
Causes and Genetic Mutations
Bartter syndrome results from changes (mutations) in genes that encode proteins essential for salt and electrolyte transport in the kidneys. These genetic mutations interfere with the kidney’s normal ability to reabsorb sodium, chloride, and other ions in key nephron segments. Five principal genes have been identified as responsible for different types of Bartter syndrome. Each gene encodes a different protein involved in the tubular reabsorption process.
| Type | Gene | Protein Function | Main Segment Affected |
|---|---|---|---|
| Type I | SLC12A1 | Na-K-2Cl cotransporter | Thick ascending loop of Henle |
| Type II | KCNJ1 | Renal outer medullary potassium channel | Thick ascending loop of Henle |
| Type III | CLCNKB | Chloride channel Kb | Loop of Henle/distal tubule |
| Type IV (A/B) | BSND, CLCNKA + CLCNKB | Barttin and related chloride channels | Thick ascending loop of Henle and inner ear |
| Other forms (rare) | MAGED2 (Type V) | Role in prenatal variant | Prenatal kidney function |
Mutations in these genes cause the kidneys to excrete excessive amounts of sodium and chloride, followed by compensatory potassium and water loss. This ultimately leads to characteristic electrolyte imbalances, including hypokalemia (low potassium), hypochloremia (low chloride), and metabolic alkalosis (increased blood pH).
In a minority of cases, the genetic cause may remain unidentified as research into additional causative genes continues.
Types and Subtypes of Bartter Syndrome
Bartter syndrome is divided into several types, each associated with a different genetic mutation and sometimes with varying severity or symptom presentation. The main recognized types include:
- Type I: Due to SLC12A1 gene mutations. Typically presents early and may show severe symptoms.
- Type II: Caused by KCNJ1 gene mutations. Also presents early, often with more prominent potassium wasting.
- Type III: From CLCNKB gene mutations. May have a later onset or milder course.
- Type IV: Associated with BSND gene or combined CLCNKA/CLCNKB mutations; often includes sensorineural hearing loss.
- Type V: Linked to MAGED2 mutations. Affects fetuses and resolves after birth in some cases.
Pathophysiology
The primary defect in Bartter syndrome is abnormal transport of sodium, potassium, and chloride ions across the thick ascending limb of the loop of Henle in the nephrons. The lack of reabsorption leads to excessive urinary loss of these ions, which the body attempts to correct through hormonal responses that unfortunately worsen potassium loss and lead to further complications:
- Salt Loss: Sodium and chloride lost via urine, leading to increased renin and aldosterone.
- Potassium Depletion (Hypokalemia): High levels of aldosterone cause further loss of potassium.
- Metabolic Alkalosis: Increased alkaline state due to shifts in acid/base and ion handling.
- Abnormal Calcium/Magnesium Handling: May lead to high urine calcium (hypercalciuria) and, in some forms, kidney stones.
Diagnosis
Diagnosing Bartter syndrome involves a comprehensive approach including:
- Medical history, especially family history and onset of symptoms
- Physical examination focusing on growth parameters and signs of dehydration or weakness
- Laboratory Testing — Typical findings:
- Low blood potassium (hypokalemia)
- Metabolic alkalosis (increased blood pH)
- High levels of renin and aldosterone hormones
- High urinary loss of potassium, chloride, and sodium
- Normal or low blood pressure
- Possible high urinary calcium (in some subtypes)
- Genetic Testing to identify causative mutations
Prenatal ultrasound may detect polyhydramnios (excessive amniotic fluid), suggestive of antenatal Bartter syndrome.
Inheritance Pattern
Bartter syndrome is inherited in an autosomal recessive pattern. This means both parents must be carriers of a mutated gene for a child to be affected. Carriers typically do not have symptoms. When both parents carry one copy of the mutated gene, each pregnancy has:
- 25% chance the child will be affected
- 50% chance the child will be a carrier
- 25% chance neither mutation will be passed on
Certain subtypes with combined gene mutations may display slightly different inheritance patterns, but the classic autosomal recessive pattern predominates.
Epidemiology and Prevalence
Bartter syndrome is considered a rare disorder. Exact prevalence is difficult to determine due to frequent underdiagnosis or misdiagnosis, but estimates suggest it affects between one in 100,000 to one in one million individuals worldwide. There is no known population predilection, and the disorder affects both males and females equally.
Risk Factors and Complications
The main risk factor is a family history of Bartter syndrome or known carrier status for the relevant gene mutations. If both parents are carriers, the risk of having an affected child increases substantially.
Potential complications, especially if untreated, include:
- Problems with growth and physical development
- Muscle paralysis due to severe electrolyte disturbances
- Kidney dysfunction or failure
- Cardiac arrhythmias (abnormal heart rhythms)
- Intellectual and developmental delays (rare)
- Sensorineural hearing loss (in some subtypes)
- Seizures
Treatment and Management
There is currently no cure for Bartter syndrome, but symptoms and electrolyte imbalances can often be effectively managed. The goal of treatment is to correct the body’s salt and potassium loss, improve growth, and minimize complications.
Typical management strategies include:
- Oral supplements (potassium, sodium, sometimes magnesium)
- Use of nonsteroidal anti-inflammatory drugs (NSAIDs) such as indomethacin, which can help reduce production of prostaglandins that worsen salt loss
- Possible use of aldosterone antagonists or potassium-sparing diuretics in select cases
- High-salt diet (especially in infants and young children)
- Regular monitoring of electrolyte levels and kidney function
In severe neonatal forms, intravenous fluids and electrolytes may be needed initially. Children with growth delays may benefit from nutritional support and close monitoring by a pediatric nephrologist. In subtypes with hearing loss, early audiology evaluation and intervention is recommended.
Long-Term Outlook
Many children with Bartter syndrome grow up to lead relatively normal lives with appropriate management, although ongoing therapy and regular laboratory monitoring are usually needed. Growth and intellectual development may normalize, though some individuals may experience persistent kidney issues or need adjustments in treatment as they age.
Can Bartter Syndrome Be Prevented?
Bartter syndrome is a genetic condition and cannot be prevented. If you have a family history of Bartter syndrome or are known to be a carrier, genetic counseling and testing can identify carrier status and inform reproductive decisions.
Other Names for This Condition
- Aldosteronism with hyperplasia of the adrenal cortex
- Bartter disease
- Bartter’s syndrome
- Juxtaglomerular hyperplasia with secondary aldosteronism
Living With Bartter Syndrome
Because Bartter syndrome is chronic, individuals and families benefit from learning to recognize symptoms of electrolyte imbalance and adhering to long-term management plans. Coordination with a healthcare team (nephrologists, pediatricians, dietitians, and genetic counselors) is essential. With modern treatments, quality of life can be significantly improved and complications minimized.
Frequently Asked Questions (FAQs)
Q: What is the life expectancy for someone with Bartter syndrome?
A: With timely diagnosis and proper management, individuals with Bartter syndrome can have a normal life expectancy. Severe untreated cases may face kidney problems or other complications.
Q: Is Bartter syndrome always inherited?
A: Yes, it is an inherited disorder caused by autosomal recessive mutations. Sometimes the exact gene mutation cannot be identified but inheritance is always genetic.
Q: Does Bartter syndrome affect cognitive function or intelligence?
A: Most individuals have normal intelligence, though severely affected infants may experience developmental delays if salt and electrolyte imbalances are prolonged and untreated.
Q: Can Bartter syndrome be detected before birth?
A: Antenatal Bartter syndrome may be suspected if prenatal ultrasound finds excessive amniotic fluid. Genetic testing can confirm the diagnosis when family history suggests risk.
Q: Is there a cure for Bartter syndrome?
A: There is no cure, but effective management of symptoms allows most individuals to have a good quality of life.
Additional Resources
- MedlinePlus Genetics
- National Organization for Rare Disorders (NORD)
- Children’s hospitals with pediatric nephrology specialists
Read full bio of medha deb












