Herniated Disk: Causes, Symptoms, Diagnosis and Treatment
Comprehensive guide on herniated disks: symptoms, causes, evaluations, treatment options, recovery, and prevention.
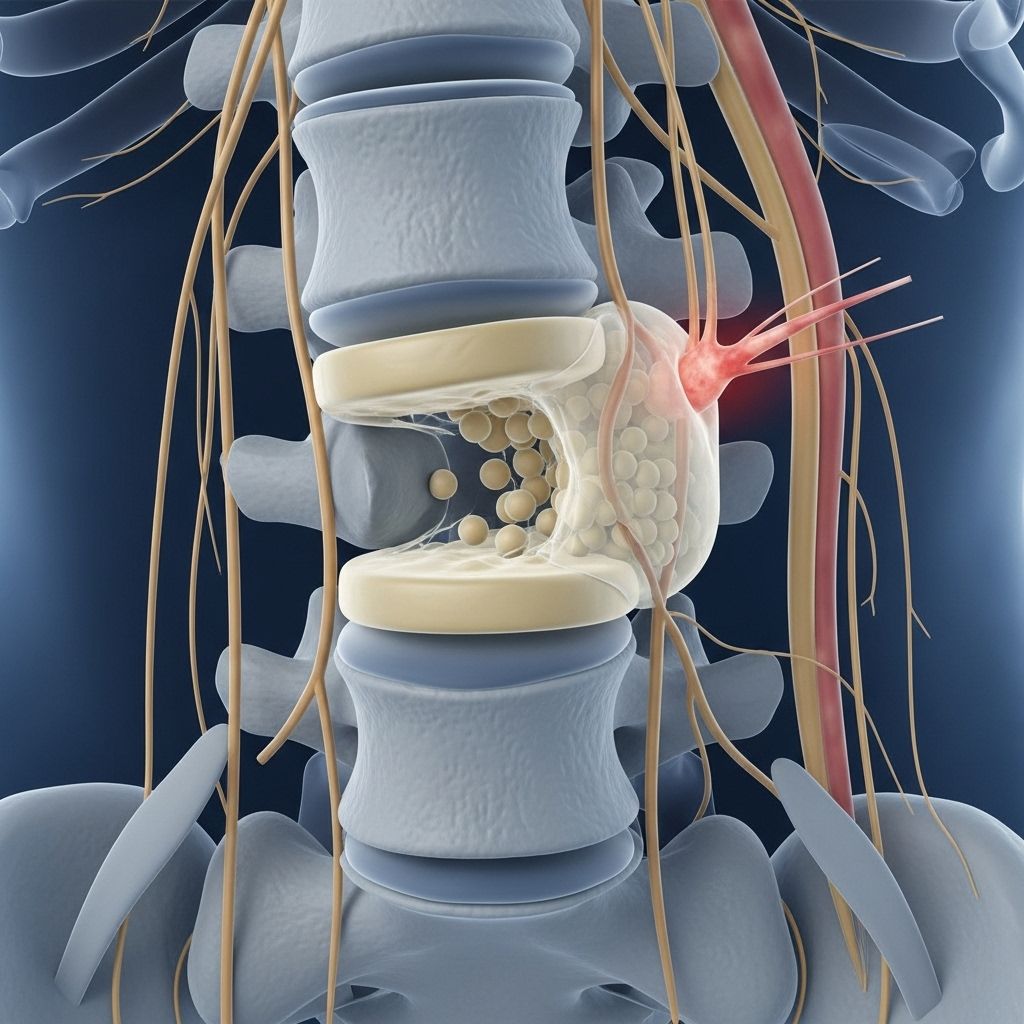
Herniated Disk: An In-Depth Overview
A herniated disk, sometimes called a “slipped” or “ruptured” disk, occurs when the soft inner portion of a spinal disk protrudes through a tear in its tough outer layer. This condition can compress nearby nerves, leading to pain, numbness, or weakness in various parts of the body. Understanding herniated disks is crucial for prompt diagnosis, effective treatment, and prevention of long-term complications.
What Is a Herniated Disk?
The spine consists of a stack of bones called vertebrae separated by intervertebral disks. These disks act as cushions and shock absorbers, helping maintain flexibility and motion in the spine. Each disk has a soft, jelly-like center called the nucleus pulposus and a tough outer ring known as the annulus fibrosus. A herniated disk develops when a portion of the nucleus pushes through a weakened or damaged area of the annulus, leading to disk material protrusion. This displacement can interfere with spinal nerves or the spinal cord itself, resulting in various symptoms depending on the location and severity.
Common Areas Affected
- Lumbar spine (lower back): The most frequently affected area, causing symptoms in the legs (sciatica).
- Cervical spine (neck): Less common, may cause pain radiating to the shoulders, arms, or hands.
- Thoracic spine (mid-back): Rarely affected but can produce symptoms in the chest or abdomen.
Causes of Herniated Disks
Multiple factors can contribute to the development of a herniated disk. Understanding these can help with both prevention and management.
- Age-related degeneration: As people age, disks lose water content, become less flexible, and are more prone to tearing or rupturing with minor strain.
- Trauma: Sudden heavy strain, a direct blow to the back, or a fall can cause a disk to herniate.
- Improper lifting techniques: Bending and twisting while lifting heavy objects places uneven pressure on the spine, increasing the risk.
- Genetic predisposition: Some individuals may inherit a tendency to develop herniated disks.
- Repetitive activities: Repeatedly performing tasks that strain the back (especially manual labor) increases risk.
- Obesity: Excess body weight can place additional stress on the spinal disks.
- Smoking: Tobacco use may decrease oxygen supply to disks, accelerating degeneration.
Symptoms of a Herniated Disk
The symptoms vary based on which part of the spine is affected and whether surrounding nerves are compressed. Many people have herniated disks without symptoms; others experience significant pain and disability.
- Pain: Often sharp or burning, localized to the back or radiating to the extremities.
- Numbness or tingling: Especially in the arms, hands, legs, or feet, depending on the location.
- Weakness: Muscles near the affected nerves may weaken, impacting movement and coordination.
- Sciatica: Shooting pain that spreads from the lower back down the leg, characteristic of lumbar disk herniation.
- Pain intensifies with movement: Activities such as bending, coughing, sneezing, or sitting for prolonged periods can worsen symptoms.
- Loss of reflexes: In advanced cases, reflexes in the knee or ankle may be diminished.
Warning Signs of Severe Complications
- Loss of control over urination or bowel movements (incontinence)
- Severe or progressive weakness in the legs or arms
- Difficulty walking or maintaining balance
Seek immediate medical attention if any of these severe symptoms develop, as they may indicate nerve damage or spinal cord compression that can be permanent if not treated promptly.
Diagnostic Evaluation
Diagnosing a herniated disk typically involves a combination of clinical evaluation and imaging studies to confirm the diagnosis and rule out other conditions.
Medical History & Physical Exam
- Assessment of symptoms, onset, and exacerbating or relieving factors
- Inspection and palpation of the spine for tenderness or swelling
- Neurological examination to assess muscle strength, sensation, and reflexes
Imaging Tests
- MRI (Magnetic Resonance Imaging): The preferred method for visualizing disks, nerves, and spinal structures.
- CT (Computed Tomography) Scan: Useful if MRI is unavailable or contraindicated.
- X-rays: Do not show herniated disks but can help rule out other causes like fractures.
- Myelogram: Involves injecting contrast dye into the spinal canal followed by X-rays or CT.
Electrodiagnostic Studies
- Electromyography (EMG) and Nerve Conduction Studies (NCS): Assess nerve function and pinpoint the exact nerves involved.
Treatment Options for Herniated Disks
Most cases of herniated disks improve without surgery. The goals of treatment focus on relieving pain, restoring function, and preventing recurrence.
1. Conservative (Non-Surgical) Treatments
- Rest: Limiting strenuous activities for a few days may help decrease symptoms, but extended bed rest is discouraged.
- Pain Medication: Over-the-counter pain relievers such as acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs) help manage pain and inflammation. Occasionally, muscle relaxants or nerve pain medications may be prescribed.
- Physical Therapy: A targeted program can help improve flexibility, strengthen the muscles supporting the spine, and teach proper movement techniques. Modalities may include:
- Stretching and strengthening exercises
- Manual therapy or soft tissue massage
- Ultrasound, electrical stimulation, or heat/cold therapies
- Epidural Steroid Injections: In select cases, corticosteroid injections near the affected nerve may reduce pain and inflammation.
- Activity modification: Avoidance of activities that exacerbate pain while maintaining as much activity as possible.
2. Surgical Treatments
Surgery is reserved for cases where conservative management fails, the patient experiences progressive neurological deficits, or there are signs of spinal cord compression.
- Discectomy (Diskectomy): The most common surgery, involving removal of all or part of the herniated disk material to relieve pressure on the nerve.
- Laminectomy: Removal of a small portion of the vertebral bone to enlarge the spinal canal and reduce nerve pressure.
- Microdiscectomy: A minimally invasive version of discectomy, using microscopic techniques.
- Spinal Fusion: In select cases where disk removal destabilizes the spine, fusion may be needed.
- Artificial Disk Replacement: For certain patients, the damaged disk may be replaced with an artificial one.
Prognosis and Recovery
The majority of people with herniated disks recover well and regain normal activities within a few weeks to months. Early treatment enhances the odds of a full recovery.
- Pain usually improves within six weeks for most individuals treated conservatively.
- Physical therapy and exercise are critical for long-term success and to prevent recurrence.
- Surgical interventions have high success rates, especially for well-selected patients, but carry some risks associated with surgery in general.
- Chronic pain or persistent weakness can occur in some cases, especially when nerve compression is severe or treatment is delayed.
Possible Complications
While most cases resolve favorably, some individuals may experience complications related to nerve damage, chronic pain, or surgical intervention.
- Chronic pain or disability
- Permanent nerve damage resulting in weakness, numbness, or loss of reflexes
- Cauda equina syndrome: Compression of nerve roots at the base of the spinal cord causing bowel or bladder dysfunction and surgical emergency
- Recurrence of herniated disk at the same or different level
- Infection or bleeding after surgery
Prevention Strategies
While not all cases can be prevented, several measures can lower the risk of disk herniation and support spinal health.
- Maintain healthy body weight to reduce stress on the spine.
- Practice proper lifting techniques: Bend at the knees, keep the back straight, and avoid twisting motions during lifts.
- Engage in regular physical activity that strengthens the core and supports spinal stability.
- Take frequent breaks from repetitive or prolonged activities, especially when sitting or standing.
- Avoid tobacco use, as it contributes to disk degeneration.
- Maintain good posture while sitting, standing, and moving.
Frequently Asked Questions (FAQs)
Q: Can herniated disks heal without surgery?
A: Yes, the majority of herniated disks improve with conservative measures such as rest, physical therapy, and medication. Surgery is only necessary in persistent or severe cases.
Q: What activities should I avoid if I have a herniated disk?
A: Avoid heavy lifting, twisting, high-impact sports, and activities that worsen your pain. Work with your healthcare provider or physical therapist to develop a safe activity plan.
Q: When is surgery recommended for a herniated disk?
A: Surgery is considered if pain persists despite several weeks of treatment, if there is significant weakness or numbness, or in emergencies (e.g., cauda equina syndrome or spinal cord compression).
Q: Can I prevent a herniated disk from recurring?
A: While recurrence cannot be completely eliminated, maintaining a healthy lifestyle, strengthening your back and core muscles, practicing good posture, and using safe lifting techniques can significantly reduce your risk.
Summary Table: Herniated Disk at a Glance
| Aspect | Description |
|---|---|
| Definition | Displacement of disk material through a tear in the outer layer of the intervertebral disk |
| Most Common Location | Lumbar (lower back) |
| Primary Symptoms | Pain, numbness, tingling, weakness |
| Key Diagnostic Tools | MRI, CT scan, EMG/NCS |
| First-line Treatment | Rest, medication, physical therapy |
| When to Consider Surgery | Persistent symptoms, neurological deficits, or emergencies |
| Prognosis | Generally good with timely management |
References
- Adapted and synthesized from authoritative medical resources and up-to-date health literature.
Read full bio of Sneha Tete












