Hip Replacement Surgery: Procedure, Recovery, and Life After
A comprehensive guide to understanding, preparing for, and recovering from hip replacement surgery, including key phases of rehabilitation, recovery tips, and FAQs.
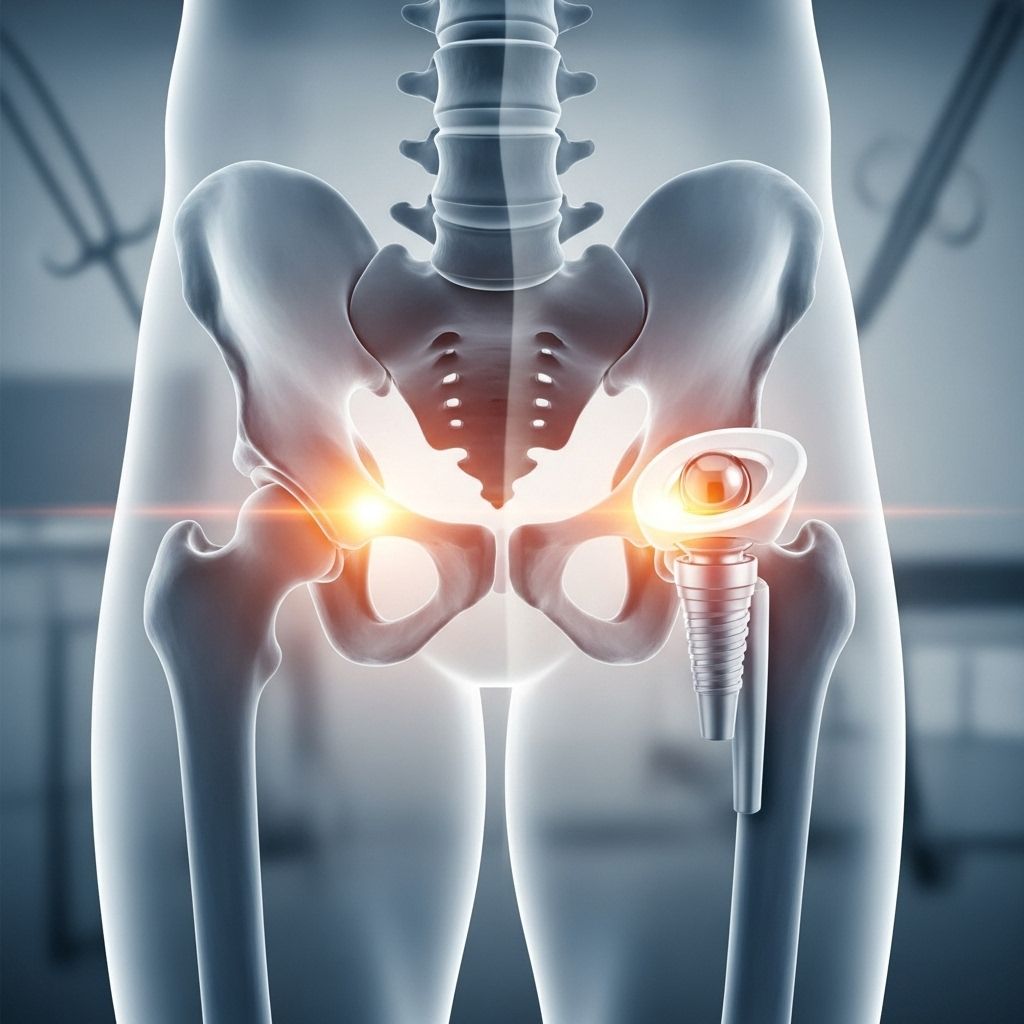
Hip Replacement Surgery Overview
Hip replacement surgery, medically termed total hip arthroplasty, is a widely performed orthopedic procedure aiming to alleviate pain and restore mobility in individuals with severe hip joint damage. The procedure involves replacing the diseased or injured parts of the hip joint with artificial components, typically made from metal, ceramic, or high-grade plastic.
The most common conditions leading to hip replacement are osteoarthritis, rheumatoid arthritis, traumatic injury, and other degenerative joint diseases.
Why is Hip Replacement Surgery Needed?
- Severe pain or stiffness: When discomfort in the hip impedes daily activities like walking, climbing stairs, or rising from a chair.
- Reduced mobility: Loss of joint movement hinders healthy, independent living.
- Other treatments have failed: Conservative interventions, such as medications, physical therapy, or minimally invasive procedures, no longer offer relief.
- Chronic inflammation and swelling: Conditions such as arthritis cause ongoing pain and joint inflammation.
Types of Hip Replacement Surgery
There are several approaches and prosthesis types used in hip replacement procedures:
- Total Hip Replacement (THR): Both the ball (femoral head) and the socket (acetabulum) of the hip joint are replaced.
- Partial Hip Replacement: Only one part, usually the femoral head, is replaced. Mostly performed in certain fracture cases.
- Revision Hip Replacement: Previous artificial hip joint is replaced with a new one due to wear, injury, or infection.
- Approaches: The surgery may use various incisions and techniques, including the traditional posterior approach or the minimally invasive direct anterior approach, which may reduce recovery times for some patients.
Preparing for Hip Replacement Surgery
Successful outcomes begin with careful preparation. Physicians will evaluate your overall health, discuss the surgical risks and benefits, and recommend preoperative exercises tailored to your level of function and pain.
Typical pre-surgery steps include:
- Reviewing medical history and preoperative assessments.
- Discontinuing certain medications as directed.
- Blood tests, imaging, and sometimes cardiac clearance.
- Strengthening and stretching exercises for muscles around the hip.
- Planning post-surgical assistance at home and ensuring accessibility (e.g., handrails, clear walkways).
The Procedure: What Happens During Surgery?
Hip replacement surgery is typically performed under general or regional anesthesia. The process usually takes a few hours and involves the following steps:
- An incision is made over the hip joint.
- The damaged bone and cartilage are removed from the joint.
- Replacement with prosthetic components: an artificial ball and socket.
- Testing joint function and ensuring stability.
- Closing the incision and applying dressings.
Most patients stay in the hospital for one to three days, though outpatient and same-day discharge options are increasingly common for healthy individuals.
Recovery After Hip Replacement Surgery
Recovery is a phased process involving careful rehabilitation and monitoring. The goals are pain management, safely restoring motion and strength, and minimizing complications. While post-surgical pain is expected initially, significant improvement is usually noted within the first two weeks, and many can walk with assistance soon after surgery.
Initial Postoperative Care
- Monitoring vital signs and surgical site to prevent infection.
- Pain control through medications as prescribed.
- Early mobilization: physical therapy often starts on the same day as surgery, with walking assistance (walker, cane, or crutches).
- Blood clot prevention: movement, compression devices, and blood thinners are often used.
Standard Recovery Timeline
| Timeframe | Expected Milestones |
|---|---|
| First 1 6 Days | Hospital stay, initial walking with support, pain management. |
| First 2 Weeks | Home recovery, begin basic exercises, monitor incision, manage swelling. |
| Weeks 2 6 | Increase walking distance, resume light activities, outpatient physical therapy. |
| Weeks 6 612 | Advanced mobility, focus on gait and strength, progress toward unassisted walking. |
| Months 3 66 | Return to many normal activities, may start sport-specific exercises, full ambulation expected. |
| 6 612 Months | Most are pain-free and resume normal routines. |
Phases of Rehabilitation
Rehabilitation is critical to a successful outcome and is organized into distinct stages:
Phase 0: Preoperative Preparation
- Education regarding surgery goals and procedure.
- Muscle strengthening and flexibility exercises.
- Preparation of home environment.
Phase I: Acute and Subacute Postoperative Recovery
- Rest and joint protection.
- Tissue healing and injury prevention.
- Initial physical therapy focusing on gentle movements and isometric exercises.
- Assisted walking, usually with a walker.
- Preventing contractures: avoid placing pillow under knee to prevent hip/knee stiffness.
Phase II: Restoring Motion and Strength
- Progress on range of motion and walking endurance.
- Strengthening hip and lower extremity muscles; core stability emphasized.
- Efforts to normalize gait, increase stride length, and cadence.
- Transition from walker to cane, then independent walking as tolerated.
- Criteria to advance: full, pain-free joint motion, sufficient muscle strength, and ability to ambulate community distances.
Phase III: Return to Function and Activity
- Focus on higher-level activities and patient-specific functional goals.
- Aerobic fitness and endurance training.
- Balance, stability, and challenging activities (including sport-specific movement if approved by surgeon).
- Duration varies, often from 12 to 24 weeks post-surgery, depending on recovery and goals.
Exercises for Hip Replacement Recovery
Following your physical therapist’s exercise regimen helps speed up recovery, restore strength, balance, and range of motion, and prevent complications.
- Ankle pumps: Move feet up and down to promote circulation.
- Quadriceps sets: Tighten thigh muscles with knee extended.
- Hip abductions: Slide leg out to the side and back.
- Gluteal sets: Tighten buttocks for muscle activation.
- Standing exercises: When cleared, practice gentle standing leg lifts, balance exercises, and walking drills.
Consistency is key for optimal recovery. Most patients are encouraged to perform their exercises for at least two months post surgery, or longer as tolerated.
Potential Risks and Complications
- Infection: Wound or implant infections may require extra treatment.
- Blood clots: Movement and medication help prevent deep vein thrombosis (DVT).
- Implant problems: Loosening or wear may necessitate revision surgery.
- Dislocation: Rare, but precautions on movement and positioning are essential.
- Nerve or blood vessel injury (rare).
- Differences in leg length: Addressed during surgery, but mild mismatches can occur.
What to Expect: Life After Hip Replacement
Most patients report significant improvement in pain and quality of life after recovery. Many resume normal activities and are pain-free within a year. The modern procedure allows for relatively quick outpatient recovery for many; some return home the same day as surgery.
- Activity: Most daily activities can resume within 3–6 months. Sports and higher impact activities are possible after consulting with your surgeon.
- Long-term care: Hip implants usually last for decades, but care is needed to avoid extreme stress or injury.
- Participation: Physical activities like walking, swimming, and cycling are generally considered safe and beneficial.
- Surveillance: Regular check-ups and imaging track implant status.
Frequently Asked Questions (FAQs)
How soon can I walk after hip replacement surgery?
Most people begin walking with the assistance of a physical therapist and support device on the same day as surgery or the next day. Walking distance and independence will gradually improve over several weeks.
Is rehabilitation always necessary after hip replacement?
Yes. Rehabilitation, either at home or outpatient therapy, is crucial for optimal healing, restoring motion, preventing complications, and guiding safe activities.
How long does recovery usually take?
The initial 2–4 weeks focus on pain control and basic mobility. Most people return to normal activities by 3–6 months, and are typically pain free within a year.
Are there things I should avoid after hip replacement?
Certain movements (bending too far, crossing legs, twisting) may risk dislocation. Your care team will provide position and movement precautions tailored to your surgery and implant type.
What are the risks of hip replacement?
Risks include infection, blood clots, implant issues, dislocation, and, less commonly, nerve or vessel injury. These risks are reduced with proper technique and rehabilitation.
How long do artificial hip joints last?
Most modern implants last 15–20 years or longer. Longevity depends on activity level, overall health, and implant type.
Tips for a Smooth Recovery
- Follow all post-surgical instructions from your care team.
- Take medications as prescribed.
- Attend physical therapy sessions consistently.
- Keep surgical site clean and dry.
- Set up a safe home environment (remove loose rugs, install handrails, etc.).
- Ask about home care services or community support if needed.
- Keep all follow-up appointments with your surgeon.
Additional Resources
- American Academy of Orthopaedic Surgeons (AAOS) – recovery guides and exercise manuals.
- Hospital for Special Surgery (HSS) – patient testimonials and rehabilitation plans.
- Brigham and Women’s Hospital – detailed recovery timelines and advice.
- Yale Medicine – physical therapy and postoperative care tips.
Read full bio of medha deb












