Meniscus Tear: Causes, Symptoms, Treatment and Recovery
Comprehensive guide to meniscus tears: symptoms, causes, diagnosis, treatment options, and long-term recovery for optimal knee health.
A meniscus tear is one of the most common knee injuries, affecting people of all ages but especially active individuals and older adults. This in-depth guide explores what a meniscus tear is, its causes, symptoms, diagnosis, treatment options—including when surgery may (or may not) be needed—and advice for long-term knee health and recovery.
What Is the Meniscus?
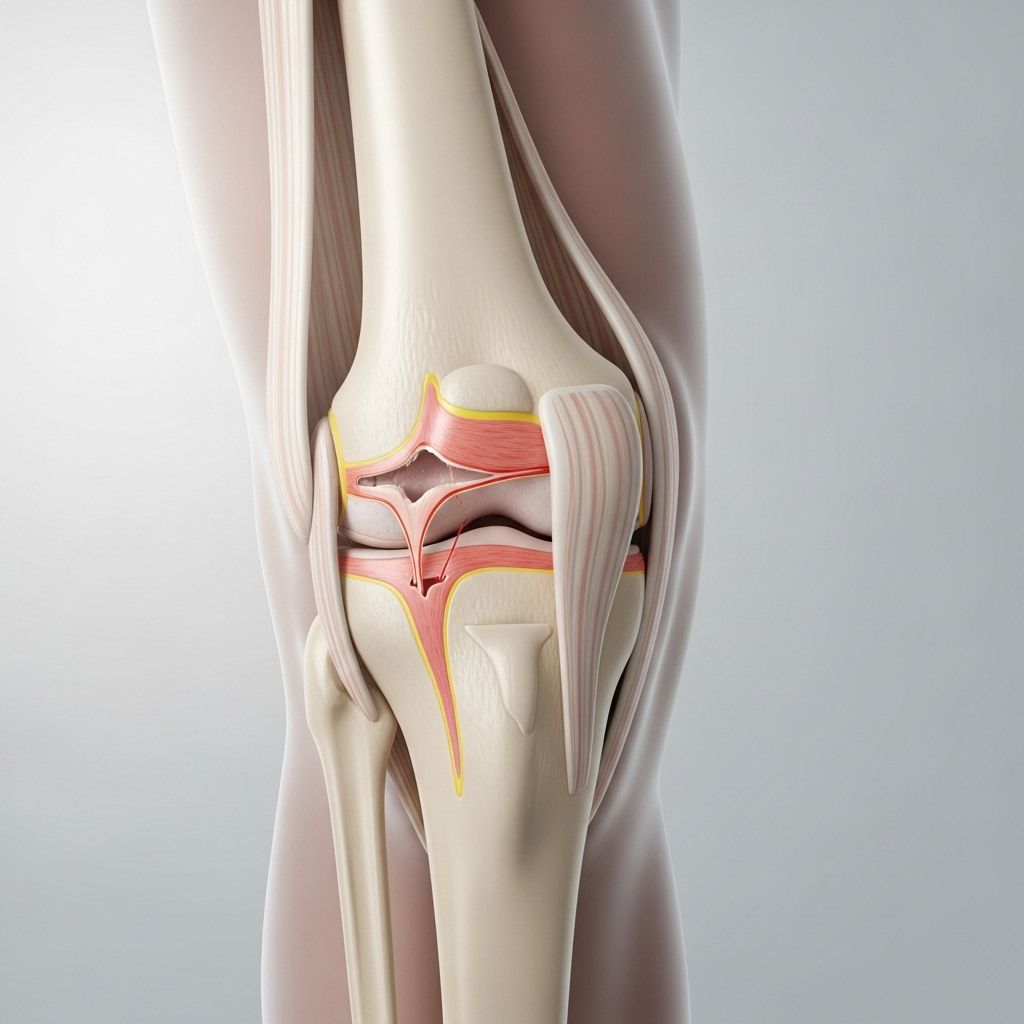
The menisci are two C-shaped pads of tough, rubber-like cartilage located between your thigh bone (femur) and shin bone (tibia) in each knee. These structures are known as the medial meniscus (inside of the knee) and the lateral meniscus (outside of the knee). Their main functions include:
- Absorbing shock from movements like walking, running, and jumping
- Improving joint stability by evenly distributing body weight across the knee
- Ensuring smooth movement of the knee joint
When this cartilage is damaged, it can disrupt normal knee mechanics and lead to pain or limited mobility.
Types and Causes of Meniscus Tears
How Do Meniscus Tears Occur?
There are two primary mechanisms by which the meniscus can be injured:
- Traumatic tears: Sudden injuries usually caused by twisting, pivoting, or forceful impact. Common in athletes and people under 40.
- Degenerative tears: Gradual wear and tear associated with aging, most common in people over 40. These tears can occur without any single, identifiable injury and are often linked to early osteoarthritis.
Types of Meniscus Tears
Meniscal tears are classified by their shape and location. The six main types include:
- Horizontal tears
- Longitudinal tears
- Radial tears
- Bucket-handle tears
- Flap tears
- Degenerative tears
Each type can affect symptoms and treatment options.
| Type | Description | Common Cause |
|---|---|---|
| Horizontal | Flat, horizontal splits in the cartilage | Degeneration with age |
| Longitudinal | Vertical tears along the length | Twisting injuries |
| Radial | Extend from inner edge outward | Trauma |
| Bucket-handle | A subtype of longitudinal, causing a fragment to displace | Acute injury |
| Flap | Partial detachments causing a ‘flap’ | Sudden trauma |
| Degenerative | Complex, frayed tears | Aging or osteoarthritis |
Risk Factors
- Age: Degenerative tears are more common in people over 40.
- Sports participation: Twisting sports (football, basketball, skiing) increase risk.
- Obesity: Extra weight places more stress on the knee.
- Past knee injuries
- Reduced flexibility or muscle weakness
Symptoms of a Meniscus Tear
The symptoms can vary depending on the type, size, and location of the tear. Common signs include:
- Pain along the knee joint line (inside or outside depending on the meniscus involved). Pain may worsen when the knee is twisted, bent, or under load (e.g., climbing stairs).
- Swelling: Often develops within 1-2 days after acute injury.
- Stiffness or loss of motion
- Clicking, popping, or catching sensations in the knee
- Knee may lock or become stuck, especially if a fragment is dislodged.
- Occasional giving way or feeling of instability
- In degenerative tears, symptoms may develop gradually with aching worsening over time. Night pain is common.
Some minor tears may cause little or no discomfort, while severe cases can be highly limiting.
When to Seek Medical Advice
Contact a GP or healthcare professional if:
- You experience severe knee pain after a twist or trauma
- There is noticeable swelling or an inability to move the knee properly
- The knee locks, buckles, or cannot bear weight
- Symptoms do not improve after a few weeks of self-care
Diagnosing a Meniscus Tear
A diagnosis is based on a combination of medical history, symptom description, and physical examination of the knee. A doctor or physiotherapist may:
- Ask about recent injuries, activities, and symptom onset
- Examine the knee for joint line tenderness, swelling, movement restriction, or mechanical symptoms (such as clicking or locking)
Imaging tests are not always required. In certain situations, an X-ray may help exclude arthritis or fractures, while an MRI can confirm a suspected meniscus tear—especially when diagnosing complex injuries or considering surgery.
- MRI is more likely to be considered if severe pain, locking, or persistent unexplained symptoms are present.
- For degenerative changes in adults over 40, knees often show meniscus changes on MRI, even in pain-free people.
Treatment Options for Meniscus Tears
Initial Self-Care and Conservative Management
Many meniscus tears—especially degenerative or small traumatic tears—heal effectively with non-surgical management. Conservative treatment is appropriate for most cases, including:
- Relative rest: Reducing activities that worsen pain, but staying active within limits. Avoid twisting, squatting, or high-impact sports until symptoms improve.
- Ice: Applying a cold pack, wrapped in a cloth, for up to 15 minutes several times a day to reduce pain and swelling. Never place ice directly on skin.
- Pain relief: Over-the-counter painkillers, such as paracetamol or ibuprofen, may be helpful. Consult a pharmacist or GP with any medication questions.
- Exercise and physiotherapy: A program of strengthening and stretching exercises targeting the quadriceps, hamstrings, and hip muscles can improve knee stability and function. Physiotherapists can individualize exercise plans.
- Weight management: Losing excess weight reduces stress on the knee and may improve recovery for overweight individuals.
- Injections: Corticosteroid injections may provide temporary pain relief in certain cases, but are not a cure and should be discussed with a clinician.
Most people improve over several weeks to months with these approaches.
When Is Surgery Needed?
Surgery is rarely required for degenerative meniscus tears. For traumatic tears—particularly those causing knee locking or inability to straighten the leg—surgical intervention may be warranted. Key points include:
- Degenerative tears: Research suggests arthroscopic surgery (keyhole surgery to trim/shave damaged meniscus) offers no long-term benefit for most patients. Removal of cartilage may increase risk of arthritis in the long term.
- Surgery is considered only if:
- There are mechanical symptoms like true locking or frequent giving way
- Non-surgical treatments have failed after 2-3 months
- Pain severely limits function and other causes have been excluded
- Procedures include:
- Meniscectomy: Removal of the torn meniscal tissue, typically used for irreparable or displaced tears
- Meniscus repair: Surgical stitching of torn sections, mostly reserved for traumatic tears in young, active patients
- Replacement or transplantation for rare, complex cases
Recovery and Rehabilitation
Most people with small or moderate meniscus tears recover well with time and structured rehabilitation.
- Symptoms often settle naturally over a few weeks to three months
- Exercise therapy is vital and shown to be more effective than surgery for most degenerative tears
- Pain and swelling gradually reduce with regular, gentle movement. Return to sports or strenuous activity should be gradual, based on specialist advice
- If surgery is needed, physiotherapy plays a key role post-operatively in restoring movement and strength
Sample Home Exercise Program
- Quadriceps setting: Tense thigh muscles and hold for 10 seconds, repeat 10 times
- Straight leg raises: Lying down, raise your leg straight, hold 5 seconds, repeat 10 times each leg
- Knee bends: Gently bend and straighten knee as pain allows
- Progress to more challenging balance and resistance exercises as symptoms improve
Consult a physiotherapist for personalized advice and progression.
Living With and Preventing Meniscus Tears
- Stay active, but avoid sudden twists and pivots in daily movements
- Maintain a healthy weight to reduce knee stress
- Strengthen lower limb muscles regularly, especially if involved in sports
- Use proper techniques and footwear during physical activity
- Warm up and stretch before exercise
- Treat underlying arthritis or joint problems with medical guidance
Potential Complications
- Persistent pain or swelling despite conservative management
- Development or progression of osteoarthritis in the knee joint
- Joint locking requiring intervention
- Reduced knee mobility or strength without adequate rehabilitation
Frequently Asked Questions (FAQs)
Q: Do all meniscus tears require surgery?
A: No. Most meniscus tears, especially degenerative ones and small traumatic tears, improve with non-surgical treatments. Surgery is reserved for persistent locking or failure of conservative management.
Q: How long does it take for a meniscus tear to heal?
A: Mild to moderate tears often heal within 6 to 12 weeks. Some pain may linger longer, but many people experience significant improvement in three months with appropriate care and exercise.
Q: What activities should I avoid with a meniscus tear?
A: Avoid twisting, deep squatting, kneeling, running, or jumping until pain has resolved and muscle strength returns. Gradually return to activities under guidance from a healthcare professional.
Q: Can a meniscus tear heal without surgery?
A: Many tears, especially those from wear and tear, can heal or become asymptomatic with exercise therapy, weight management, and self-care.
Q: Will a meniscus tear cause permanent knee damage?
A: Not all meniscus tears cause lasting knee problems. However, large or untreated tears and extensive cartilage removal in surgery can increase the risk of developing osteoarthritis over time.
Key Takeaways
- Meniscus tears are a common source of knee pain and dysfunction
- Most tears do not require surgery and respond well to rest, exercise, and simple pain relief
- Contact your healthcare provider if symptoms are severe, persistent, or associated with true knee locking
- Long-term recovery hinges on muscle strength, weight control, and exercise
If you are unsure about your symptoms or recovery, seek advice from your doctor or physiotherapist. Early intervention and proper management can help you regain safe, comfortable knee function.
Read full bio of medha deb












