Pancreatitis: Causes, Symptoms, Diagnosis, and Treatment
Learn about pancreatitis, its causes, symptoms, diagnosis, complications, treatment and pain management strategies from a clinical perspective.
What Is Pancreatitis?
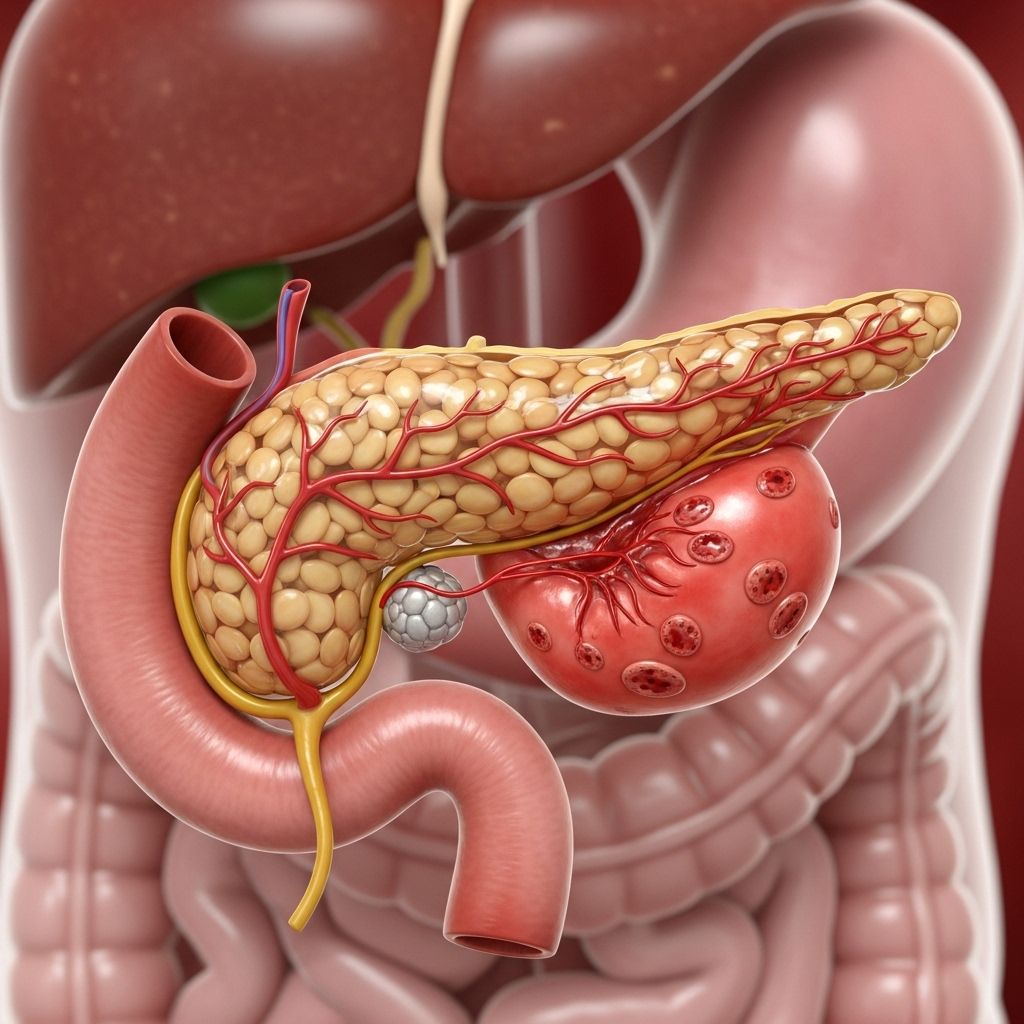
Pancreatitis is the medical term for inflammation of the pancreas, a critical organ located behind the stomach responsible for both digestive and hormonal functions. The pancreas produces digestive enzymes to help break down food as well as hormones like insulin and glucagon to regulate blood sugar levels. When the pancreas becomes inflamed, its function can be disrupted, sometimes causing serious health issues if left untreated.
Pancreas: Location and Role
The pancreas is a long, flat gland tucked behind the stomach in the upper abdomen. It has two chief roles:
- Digestive Function: Releasing enzymes into the small intestine to break down fats, proteins, and carbohydrates.
- Endocrine Function: Producing hormones (insulin and glucagon) that help control blood sugar levels.
Types of Pancreatitis
Pancreatitis can be acute or chronic. These forms have different causes, clinical presentations, and treatments.
| Type | Description | Duration |
|---|---|---|
| Acute Pancreatitis | Sudden inflammation that usually resolves with appropriate medical care; might be mild or severe | Few days to a few weeks |
| Chronic Pancreatitis | Long-lasting inflammation leading to permanent damage, impairment of pancreatic function, and often persistent pain | Months to years, with progression over time |
Acute Pancreatitis
Acute pancreatitis is a sudden and severe inflammation of the pancreas. Most people recover fully with treatment, but the condition can lead to serious complications if not managed properly. Symptoms are often abrupt, severe, and may warrant urgent care.
Chronic Pancreatitis
Chronic pancreatitis develops gradually, with ongoing inflammation causing irreversible changes to pancreatic tissue. Over time, this can reduce enzyme and hormone output, leading to digestion issues and sometimes diabetes. Persistent or recurrent pain is common.
Causes and Risk Factors
Multiple underlying conditions and lifestyle factors can trigger pancreatitis. Some of the most common include:
- Gallstones: The leading cause of acute pancreatitis. Gallstones can block the pancreatic duct, causing enzymes to back up and damage pancreatic tissue.
- Alcohol Use: Heavy and prolonged alcohol consumption is a principal cause of chronic pancreatitis and also contributes to acute cases.
- Certain Medications: Some drugs can trigger pancreatitis as a rare side effect.
- High Calcium Levels (Hypercalcemia): Often a result of overactive parathyroid glands.
- High Blood Fat Levels (Hypertriglyceridemia): Severe elevations of blood triglycerides can inflame the pancreas.
- Infections: Viral, bacterial, or parasitic infections are rare causes.
- Abdominal Trauma: Direct injury to the pancreas may induce inflammation.
- Genetic Factors: Some hereditary conditions increase susceptibility to chronic pancreatitis, such as cystic fibrosis.
Symptoms of Pancreatitis
The hallmark symptom of pancreatitis is abdominal pain, but other signs may also be present. Common symptoms include:
- Severe upper abdominal pain, which often radiates to the back
- Pain that may get worse after eating, especially high-fat meals
- Nausea and vomiting
- Fever
- Rapid pulse
- Swollen and tender abdomen
- Loss of appetite
- Unintended weight loss (more common with chronic pancreatitis)
- Diarrhea or oily, foul-smelling stools (due to poor digestion)
How Pancreatitis Is Diagnosed
Diagnosis begins with a thorough assessment of symptoms and risk factors, followed by physical examination and laboratory and imaging tests. Major steps include:
- Medical History and Exam: Detailing the pain’s location, onset, and relationship to meals and alcohol use; checking for fever, abdominal tenderness, and signs of dehydration.
- Blood Tests: Key lab markers include elevated pancreatic enzymes (amylase and lipase), increased white blood cell count and signs of inflammation.
- Imaging Studies:
- Ultrasound: Used to detect gallstones and swelling of the pancreas.
- CT Scan (Computed Tomography): Provides detailed images, identifies complications such as fluid collections, necrosis, or pseudocysts.
- MRI (Magnetic Resonance Imaging): Useful for further assessment, especially ductal abnormalities.
- Endoscopic Ultrasound (EUS) and ERCP (Endoscopic Retrograde Cholangiopancreatography): Specialized techniques to evaluate and treat ductal obstructions or strictures.
Potential Complications
Pancreatitis can range from mild to life-threatening. Significant complications can include:
- Pseudocysts: Fluid-filled sacs that can become infected or rupture
- Pancreatic Necrosis: Destruction of pancreatic tissue, increasing infection risk
- Infection/Abscess: Can require drainage or surgery
- Chronic Pain: Especially in chronic pancreatitis
- Nutrition Problems: Malabsorption of food, leading to weight loss and vitamin deficiencies
- Diabetes: Destruction of insulin-producing cells
- Systemic Complications: Such as kidney failure, respiratory distress, or shock (in severe cases)
Treatment and Management
The treatment for pancreatitis depends on its cause, severity, and complications. Goals include relieving symptoms, supporting pancreatic function, and preventing recurrence.
Immediate Treatment for Acute Pancreatitis
- Hospitalization: Most cases require admission for supportive care.
- Fasting: Oral intake is stopped to rest the pancreas. Nutrition is maintained via intravenous fluids.
- Intravenous Fluids (IV): Prevent dehydration and support circulation.
- Pain Control: Analgesics manage severe pain; options include acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), or, for severe cases, opioids as prescribed by the physician.
- Treating Underlying Cause: For example, removing gallstones via endoscopic or surgical procedures, or discontinuing an offending medication.
- Antibiotics: Only if infection is suspected or confirmed.
Long-Term Management for Chronic Pancreatitis
- Pain Management: See pain management section below for details.
- Enzyme Replacement Therapy: Oral pancreatic enzymes help with digestion when the pancreas has lost its ability to produce sufficient enzymes.
- Insulin Therapy: If diabetes develops, insulin is needed to manage blood sugar.
- Dietary Changes: Low-fat, nutrient-rich, smaller meals; avoiding alcohol and smoking is crucial.
- Surgery or Endoscopic Procedures: May be needed for persistent symptoms, duct blockages, or complications such as pseudocysts or strictures.
- Vitamin Supplementation: Especially fat-soluble vitamins (A, D, E, K) due to absorption issues.
Pain Management in Pancreatitis
Pain is often a dominant and challenging symptom, especially in chronic pancreatitis. Management involves a combination of therapies:
- Medications:
- Analgesics: Acetaminophen, NSAIDs, opioids in refractory cases
- Neuromodulators: Certain antidepressants or antiseizure drugs may help with nerve pain
- Novel options (being researched): Ketamine, lidocaine infusion, spinal cord stimulation, and endoscopic interventions
- Procedural Interventions:
- Nerve blocks (celiac plexus block)
- Endoscopic or surgical procedures to relieve duct blockages
- Spinal cord stimulation for severe, treatment-resistant pain
- Multidisciplinary Care: Combining medical, psychiatric, gastroenterological, and nutritional expertise to address both the physical and psychological impact of chronic pain
- Psychological Support: Counseling, cognitive-behavioral therapy, and support groups can improve coping and quality of life
Prevention of Pancreatitis
Some forms of pancreatitis can be prevented or have their risk reduced by addressing underlying factors:
- Limiting alcohol consumption or abstaining from alcohol altogether
- Maintaining a healthy diet low in saturated fats
- Treating gallbladder disease promptly
- Managing triglyceride and calcium levels through diet, exercise, and medication if needed
- Avoiding medications known to cause pancreatitis when possible
- Genetic counseling for hereditary pancreatitis cases
Living with Pancreatitis
Chronic pancreatitis can significantly impact quality of life through recurrent pain, digestive challenges, and increased risk of diabetes. Strategies that can help include:
- Adhering to treatment and dietary recommendations
- Regular follow-up with healthcare providers, including nutrition specialists and pain management experts
- Participating in psychosocial support and patient advocacy groups
- Monitoring for complications such as diabetes or malnutrition
Frequently Asked Questions (FAQs)
Q: What is the most common cause of acute pancreatitis?
A: Gallstones are the most frequent cause, followed closely by heavy alcohol use.
Q: Can pancreatitis be cured?
A: Acute pancreatitis can often be cured, especially when the cause is reversible. Chronic pancreatitis cannot be cured but can be managed with ongoing medical care to alleviate symptoms and prevent complications.
Q: What foods should be avoided with pancreatitis?
A: Foods high in fat, fried foods, alcohol, and processed foods should be avoided. A diet focused on lean protein, whole grains, fruits and vegetables is best for pancreas health.
Q: How is chronic pancreatitis pain managed?
A: Pain management can include medications, nerve blocks, spinal cord stimulation, enzyme replacement, and a multidisciplinary care approach that may involve pain specialists, psychiatrists, and gastroenterologists.
Q: Does pancreatitis increase diabetes risk?
A: Yes. Chronic pancreatitis can damage the insulin-producing cells of the pancreas, leading to diabetes in a significant number of patients over time.
When to See a Doctor
Anyone experiencing sudden, severe upper abdominal pain—especially if it radiates to the back, is accompanied by vomiting, or persists for several hours—should seek prompt medical attention. Early diagnosis and management are crucial for the best outcomes.
Read full bio of Sneha Tete












