Reverse Total Shoulder Replacement: Procedure, Recovery, and Risks
Discover how reverse total shoulder replacement restores mobility and relieves pain when standard shoulder surgery isn’t an option, especially for severe rotator cuff injuries.
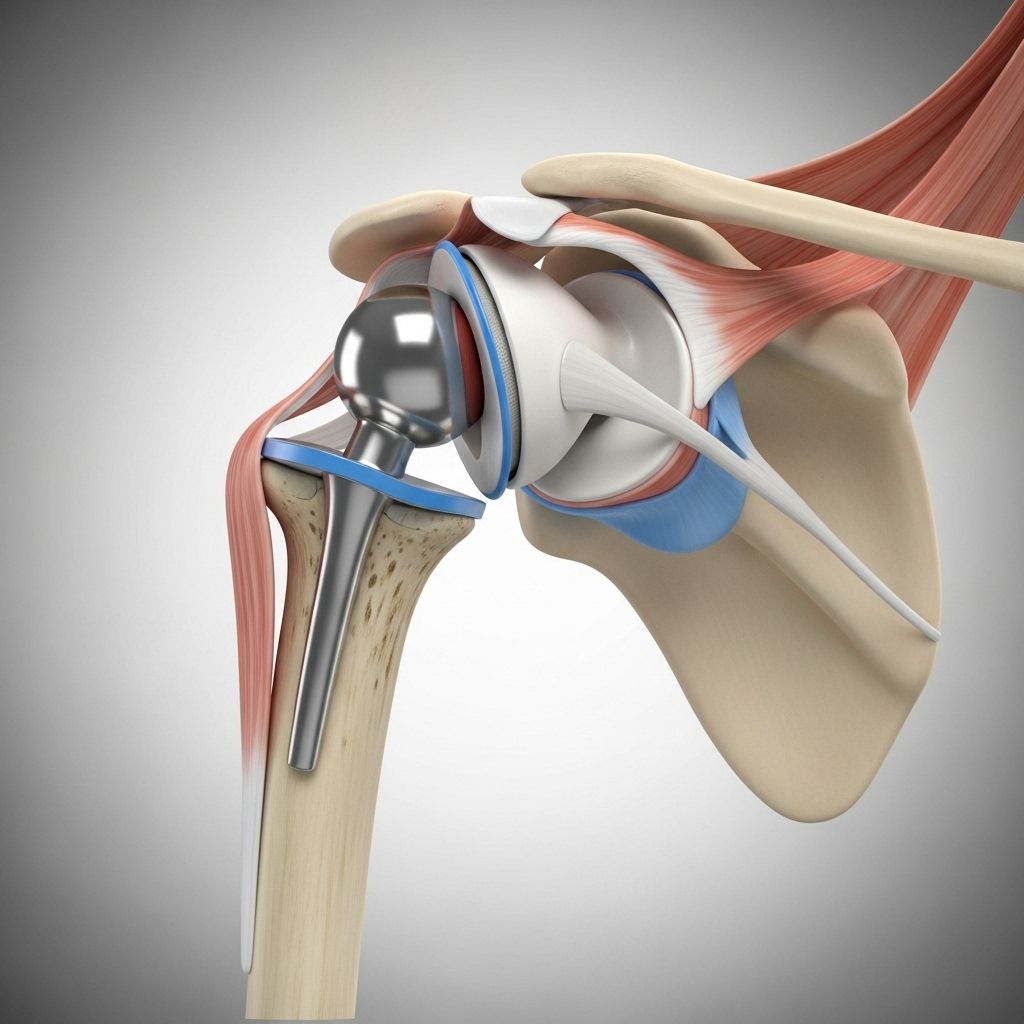
Reverse Total Shoulder Replacement
Reverse total shoulder replacement is a specialized surgical option for individuals with complex shoulder problems, particularly those with severe rotator cuff tears that cannot be repaired using traditional methods. When conventional shoulder replacement or other treatments fail to relieve pain and restore function, this innovative procedure offers an effective alternative for improving mobility and quality of life.
What Is a Reverse Total Shoulder Replacement?
Reverse total shoulder replacement, sometimes called reverse shoulder arthroplasty, is a surgery that replaces the damaged parts of the shoulder with artificial components arranged in a reverse configuration. Unlike a standard (anatomic) shoulder replacement, where the ball is placed on the upper arm bone and the socket on the shoulder blade, the reverse procedure switches their positions: the metal ball is attached to the shoulder blade (glenoid), and the plastic socket is placed on top of the arm bone (humerus).
This unique design enables the deltoid muscle—the large outer muscle of the shoulder—to move the arm, making up for non-functioning or torn rotator cuff muscles. As a result, patients with rotator cuff arthropathy (shoulder arthritis with a major rotator cuff tear) or other complex shoulder conditions can regain motion and reduce pain.
How the Shoulder Works
The shoulder is a complex ball-and-socket joint made up of three bones:
- Humerus (upper arm bone)
- Scapula (shoulder blade)
- Clavicle (collarbone)
The head of the humerus fits into a rounded socket called the glenoid on the scapula. The rotator cuff—a group of muscles and tendons surrounding the shoulder—keeps the arm centered in the socket and allows for a wide range of motion. Injury, arthritis, or severe damage to these tendons can disrupt this mechanism, leading to pain, weakness, and restricted movement.
Who Is a Candidate for Reverse Shoulder Replacement?
The procedure is typically recommended for people who have:
- A completely torn rotator cuff that cannot be repaired
- Rotator cuff tear arthropathy (arthritis coupled with rotator cuff damage)
- Unsuccessful previous shoulder replacement
- Irreparable fractures of the shoulder joint
- Chronic shoulder dislocation or instability
- Specific shoulder tumors that necessitate joint reconstruction
- Severe, persistent pain and difficulty with shoulder movement after other therapies have failed
Reverse total shoulder replacement is not typically the first choice for shoulder problems. Doctors usually recommend it when conservative treatments—such as medication, physical therapy, rest, or corticosteroid injections—do not lead to improvement, and when less complex surgical repairs are not possible or have failed.
How Does a Reverse Shoulder Replacement Differ from a Standard Shoulder Replacement?
Standard shoulder replacement—also called anatomic replacement—mimics the shoulder’s natural structure. It replaces:
- The ball (head of humerus) with a metal ball
- The socket (glenoid) with a plastic cup
This option depends on healthy rotator cuff muscles to keep the artificial joint stable and moving smoothly. If the rotator cuff is torn beyond repair, the joint may remain unstable and weak, and the implant might loosen or fail.
Reverse total shoulder replacement inverts the configuration:
- The metal ball is attached to the shoulder blade (scapula)
- The plastic socket is placed on the top part of the upper arm bone (humerus)
This arrangement shifts the movement and stabilization function to the deltoid muscle, which is usually intact even when the rotator cuff has been lost. As a result, patients can often lift and move their arms more effectively after reverse shoulder replacement, even if their rotator cuff is irreparably damaged.
Preparing for Reverse Total Shoulder Replacement Surgery
You will receive a thorough evaluation before scheduling surgery. Preparations may include:
- Physical examination and assessment of shoulder mobility and strength
- Imaging studies such as X-rays, CT scans, or MRI to evaluate bone and soft tissue
- Review of your medical history, including any chronic illnesses, medications, and allergies
- Discussion of anesthesia options, surgical risks, and postoperative expectations
- Guidance on stopping certain medications (like blood thinners) ahead of the procedure
- Instructions about fasting and logistics for the day of surgery
- Arrangements for assistance at home during the initial recovery period
The Reverse Total Shoulder Replacement Procedure: Step by Step
- Anesthesia: The procedure is performed under general anesthesia, ensuring you remain asleep and pain-free throughout the operation.
- Incision: The surgeon makes an incision on the front (or sometimes the top) of the shoulder to access the joint.
- Exposure: Muscles and soft tissue are gently separated to expose the damaged shoulder joint.
- Removal of Damaged Tissue: The damaged head of the humerus is removed, and the socket (glenoid) is prepared.
- Implant Placement:
- A flat metal baseplate is attached to the glenoid (shoulder socket) using screws.
- A smooth metal ball (glenosphere) is fitted onto this baseplate.
- The humeral canal is shaped and prepared.
- A metal stem is inserted down the humerus and topped with a plastic cup (the new artificial socket).
- The plastic socket fits securely onto the metal ball attached to the shoulder blade, reversing the normal joint configuration.
- Closure: Soft tissues are reapproximated and the incision is closed with sutures or staples.
- Recovery Room: The patient is monitored as the anesthesia wears off.
What to Expect During Recovery
Initial recovery generally begins in the hospital, where most patients remain one to two days after surgery. Common aspects of early recovery include:
- Pain management: Medication will be prescribed to control pain and inflammation.
- Arm immobilization: You will need to wear a sling to support the arm and protect the new joint for several weeks.
- Wound care: Keep the incision clean and dry. Instructions will be provided for changing dressings and caring for the wound.
- Physical therapy: Gentle exercises begin soon after surgery to maintain joint flexibility and prevent stiffness. Structured rehabilitation programs help strengthen the deltoid and shoulder muscles and gradually restore shoulder function.
- Follow-up appointments: Your physician will monitor healing and implant function through regular check-ups and imaging studies.
Full recovery can take up to six months. During this period:
- Avoid heavy lifting, pushing, or pulling with the affected arm
- Delay overhead activities and strenuous tasks until cleared by the surgeon
- Gradually increase activity level as strength and function return through therapy
Expected Benefits and Outcomes
Many patients experience substantial improvement after reverse total shoulder replacement, including:
- Significant pain relief, even in cases of chronic or severe discomfort
- Improved shoulder mobility and the ability to perform day-to-day activities, such as dressing, grooming, and reaching overhead
- Increased strength in the shoulder and arm due to reliance on the deltoid muscle
- Better overall quality of life for individuals previously limited by shoulder dysfunction
Risks and Potential Complications
As with any major surgical procedure, reverse total shoulder replacement carries some risks. While most surgeries are successful, potential complications may include:
- Infection at the surgical site
- Dislocation or instability of the new joint components
- Fracture of the humerus or scapula during or after surgery
- Nerve or blood vessel injury
- Blood clots (deep vein thrombosis)
- Wound irritation or problems with healing
- Differences in arm length
- Loosening or wearing out of the implant over time
- Prosthesis-related mechanical problems, including noise or stiffness
Your surgical team will explain these risks in detail and discuss ways to minimize complications, including the importance of following postoperative instructions carefully.
Alternatives to Reverse Shoulder Replacement
Depending on your diagnosis and overall health, alternatives may include:
- Physical therapy and rehabilitation aimed at strengthening the shoulder
- Medications and steroid injections to control pain and inflammation
- Arthroscopic repairs for certain soft tissue injuries
- Standard total shoulder replacement, if the rotator cuff is intact
- Shoulder fusion (arthrodesis) in severe cases with extensive bone or soft tissue loss
Your orthopedic surgeon will recommend the best course of action based on your condition, goals, and lifestyle.
Living With a Reverse Shoulder Replacement
The artificial components used in reverse total shoulder replacement are designed to be durable, but they may gradually wear down over time, particularly with heavy or repetitive activity. Most patients can expect the implant to last at least 10 to 20 years.
Tips for maintaining your shoulder replacement include:
- Adhering to recommended activity restrictions to avoid excessive stress on the joint
- Participating in regular follow-up visits for monitoring implant condition
- Continuing prescribed exercises to preserve flexibility and strength
- Reporting any changes in pain, function, or sensation to your healthcare provider right away
Frequently Asked Questions (FAQ)
How long does recovery take after reverse total shoulder replacement?
Most patients recover significantly within three to six months, but some improvement can continue for up to a year. Physical therapy is essential during this period to achieve the best possible function.
Will I regain full range of motion?
Many people experience good improvement in range of motion and strength, especially with daily activities like reaching and lifting. However, extreme overhead motion or heavy lifting may not return to pre-injury levels.
Is the procedure painful?
You may experience pain and discomfort immediately after surgery, which is managed with medications. Most post-surgical pain usually improves significantly within a few weeks.
What are the main risks or complications?
The most common risks include infection, dislocation, nerve injury, blood clots, and mechanical problems with the implant. Your medical team takes precautions to minimize these and will monitor you during recovery.
How soon can I get back to daily activities?
Gentle daily activities can be resumed after a few weeks, but tasks involving lifting, pushing, or pulling should be delayed for several months. Your surgeon or physical therapist will provide a graduated plan.
What is the lifespan of a reverse shoulder implant?
Most reverse shoulder implants last 10–20 years or longer, depending on patient factors and activity levels. Regular checkups are important for monitoring the implant’s condition.
Summary Table: Reverse vs. Standard Shoulder Replacement
| Feature | Standard Shoulder Replacement | Reverse Shoulder Replacement |
|---|---|---|
| Design | Metal ball on humerus, plastic socket on scapula | Metal ball on scapula, plastic socket on humerus |
| Indications | Intact rotator cuff, degenerative arthritis, fracture | Irreparable rotator cuff tear, cuff tear arthropathy |
| Primary muscle used | Rotator cuff | Deltoid |
| Stability | Dependent on healthy rotator cuff | Stable even with rotator cuff loss |
| Range of motion outcomes | Better if rotator cuff is intact | Better in rotator cuff-deficient shoulders |
If you have ongoing shoulder pain, weakness, or difficulty with movement, talk to an orthopedic specialist. Reverse total shoulder replacement offers a tailored solution for specific problems, particularly for those who have limited options due to rotator cuff injuries or past failed surgeries.
Read full bio of medha deb












