Understanding Root Canals: Procedure, Recovery, and FAQs
Comprehensive guide to root canal treatments: procedure steps, recovery, risks, expectations, and frequently asked questions.
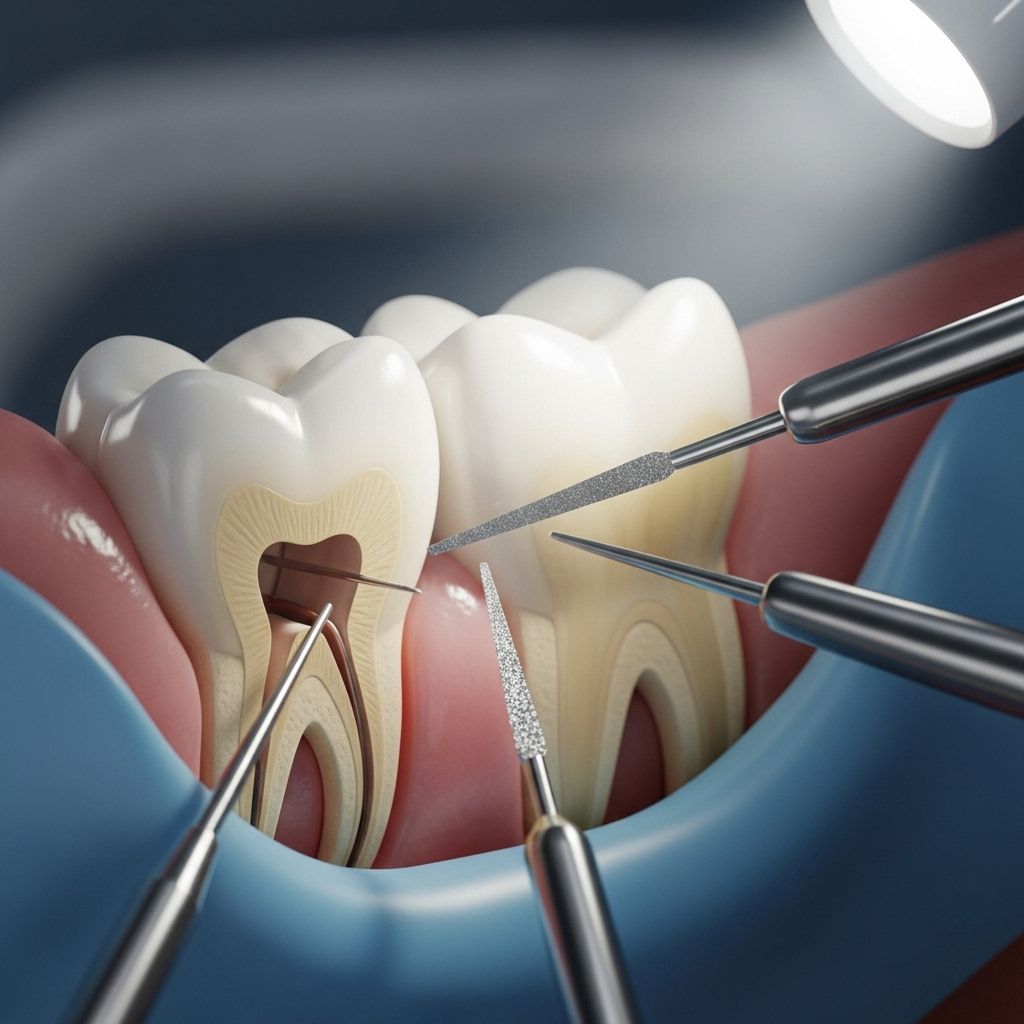
Root Canal Treatments: What You Need to Know
Root canal treatments are widely used dental procedures designed to save natural teeth that have become infected or severely decayed. Modern techniques and anesthesia make root canals a straightforward and effective procedure, aiming to relieve pain, stop tooth loss, and prevent further oral health complications. This guide explains what a root canal is, why and when this therapy is needed, the steps involved, what to expect during and after the procedure, potential risks, and essential aftercare tips.
What is a Root Canal?
A root canal is a procedure intended to treat infection or damage at the center of a tooth (the dental pulp). During the treatment, the infected or inflamed pulp is removed, the interior of the tooth is cleaned and disinfected, then filled and sealed with a material called gutta-percha. Afterwards, the tooth is restored with a filling or crown. The term “root canal” also refers to the natural cavity within the center of a tooth that houses the pulp—composed of nerves, connective tissue, and blood vessels.
- Pulp: Soft tissue inside the tooth that can become infected or inflamed due to deep decay, repeated dental procedures, cracks, chips, or trauma.
- Endodontist: A dentist with specialized training in root canal therapy and other procedures dealing with the tooth pulp and roots.
Why Might You Need a Root Canal?
Root canals become necessary when the pulp inside a tooth is infected, inflamed, or injured. Common situations that can lead to this need include:
- Deep decay or cavities reaching the pulp.
- Repeated dental treatments or procedures on the same tooth.
- Cracks or chips in the tooth exposing pulp tissue.
- Severe trauma or injury to the mouth.
- Large fillings replacing extensive decay.
Signs and Symptoms Indicating a Possible Root Canal Need
- Severe tooth pain when chewing or applying pressure.
- Prolonged sensitivity to hot or cold, even after the source is removed.
- Darkening or discoloration of the tooth.
- Swelling or tenderness in nearby gums or jaw.
- Pimple-like bump on the gums near the affected tooth (dental abscess).
However, sometimes there are no symptoms at all. Only a dental professional, using clinical examination and X-rays, can accurately determine if a root canal is required.
How is the Root Canal Procedure Performed?
The root canal process is typically completed in one or two appointments and involves several methodical steps to ensure the tooth is thoroughly cleaned and sealed. Below is a step-by-step description:
Step-by-Step Guide to a Root Canal Procedure
- Examination and X-rays
The dentist or endodontist first reviews X-rays of the affected tooth to assess the extent of infection and root canal structure. A thorough examination also takes place to plan the procedure. - Local Anesthesia
A local anesthetic is administered to numb the tooth and surrounding area, ensuring a painless experience. Sometimes, sedation or anti-anxiety medication is offered for relaxation. - Isolation with Dental Dam
A thin rubber sheet (dental dam) is placed over the area to keep the tooth dry and free of saliva throughout the treatment, as well as to prevent contamination and protect nearby tissues. - Access Opening
Using a dental drill, the dentist creates a small opening in the crown (top) of the tooth to access the pulp chamber and root canals. - Pulp Removal
The diseased or dead pulp tissue is carefully extracted from the pulp chamber and root canals using specialized instruments. - Cleaning and Shaping
The interior space is meticulously cleaned, disinfected with antiseptic solutions, and shaped with tiny files to remove any debris and create room for filling. - Filling the Root Canals
Once the canals are cleaned and dried, they are filled and sealed with a biocompatible material, usually gutta-percha. This step prevents reinfection and restores the integrity of the tooth. - Temporary or Permanent Filling/Crown
A temporary filling is often placed to protect the opening between appointments. If the tooth is restored immediately, a permanent filling or crown may be fitted to restore full function and appearance. - Final Restoration
In a subsequent visit, a permanent crown or filling replaces the temporary restoration. This adds strength, protects the tooth from future damage, and restores aesthetics.
| Step | Description |
|---|---|
| 1. Examination & X-rays | Assessment of the tooth and root structure, diagnosis of infection. |
| 2. Anesthesia | Local anesthetic administered for a painless procedure. |
| 3. Dental Dam | Rubber dam isolates the tooth for protection and cleanliness. |
| 4. Access Opening | Hole is drilled to access pulp chamber and canals. |
| 5. Pulp Removal | Removal of infected or dead pulp tissue from the tooth. |
| 6. Cleaning & Shaping | Cleaning with solutions and shaping canals for filling. |
| 7. Filling | Canals filled and sealed with gutta-percha. |
| 8. Temporary Filling | Placement of temporary restoration if final crown not ready. |
| 9. Permanent Restoration | Final filling or crown applied and adjusted. |
Does a Root Canal Hurt?
Thanks to modern anesthetics and advanced dental techniques, most patients report that having a root canal feels similar to getting a cavity filled. While some discomfort or sensitivity may occur once the anesthesia wears off, this is usually mild and temporary. Severe pain or prolonged discomfort after the procedure could indicate a complication—contact your dentist if this occurs.
Risks and Benefits of Root Canal Therapy
Benefits
- Saves a natural tooth—no need for extraction and replacement.
- Relieves tooth pain caused by infection or inflammation.
- Restores normal biting force and chewing capability.
- Protects neighboring teeth from excessive wear or strain.
- Helps maintain natural appearance and alignment of your smile.
Risks and Complications
- Possibility of a persistent or returning infection, requiring retreatment.
- Rare risk of undetected fracture or missed canal leading to failed healing.
- Tooth fracture if not properly restored with a crown or permanent filling.
- Temporary sensitivity or discomfort following the procedure.
Root canals are highly successful and have a success rate over 90%, especially when performed by an experienced dentist or endodontist. If a root canal fails, options include retreatment, endodontic surgery, or, rarely, extraction.
How to Prepare for a Root Canal
- Take all prescribed medications as directed.
- Eat a light meal beforehand, as your mouth will be numb for some time after the procedure.
- Avoid alcohol and tobacco before the appointment, which can interfere with healing.
- Discuss any allergies or medical conditions with your dentist.
Recovery After a Root Canal
Healing and return to normal activity are generally rapid after root canal treatment. Here’s what you can anticipate and do to streamline your recovery:
- Wait for numbness to wear off before eating to avoid biting your tongue or cheek.
- Take over-the-counter pain relievers or medications as prescribed.
- Avoid chewing or biting on the treated tooth until it’s fully restored.
- Maintain good oral hygiene: brush and floss as usual to prevent further decay.
- Watch for signs of complications, such as increasing pain, swelling, or allergic reactions, and contact your dentist if they occur.
- Attend all follow-up appointments to complete permanent restoration and ensure proper healing.
What to Expect Post-Procedure
- Mild soreness or sensitivity for a few days is common.
- Swelling or bruising is rare, but possible.
- Most people return to normal activities by the next day.
Prevention: Keeping Your Teeth Healthy
While root canals are effective at saving damaged teeth, prevention remains the best approach. You can reduce your risk of serious decay or infection by:
- Brushing teeth twice daily with fluoride toothpaste.
- Flossing every day to remove food particles and bacteria.
- Visiting your dentist regularly for exams and cleaning.
- Treating cavities, broken teeth, or gum disease promptly.
- Wearing a mouthguard during sports to prevent trauma.
- Avoiding chewing on hard foods, like ice and candies, or opening packages with your teeth.
Frequently Asked Questions (FAQs) About Root Canals
Q: How do I know if I need a root canal?
A: Only a dentist or endodontist can definitively diagnose the need for a root canal. Warning signs include severe pain, lingering sensitivity to heat or cold, swelling, tenderness, or a darkened tooth, but sometimes there are no clear symptoms.
Q: Is a root canal better than extracting the tooth?
A: Preserving a natural tooth through root canal therapy is typically preferable for oral health, function, and aesthetics. Extractions may require further dental work, like bridges or implants, and can cause the adjacent teeth to shift.
Q: How long does a root canal procedure take?
A: Most root canal treatments take about 60 to 90 minutes per tooth, and may require one or two visits depending on complexity and the degree of infection.
Q: Are there alternatives to root canal therapy?
A: The only alternative to root canal treatment for a severely infected or damaged tooth is extraction, which is avoided whenever possible to preserve natural chewing and bone structure.
Q: What happens if I don’t get a root canal?
A: Untreated dental infections can lead to worsening pain, abscess, jawbone loss, damage to surrounding teeth, and potentially serious systemic health problems.
Q: How long will my tooth last after a root canal?
A: Teeth treated with root canal therapy and properly restored can last a lifetime with good oral hygiene and regular dental checkups.
Q: Is there special care required after a root canal?
A: Initial care includes avoiding very hard or chewy foods until the tooth is fully restored. Long term, maintain standard oral hygiene and see your dentist regularly.
When to Call the Dentist
- Severe or worsening pain several days after the procedure.
- Noticeable swelling in your jaw or face.
- Persistent fever or signs of infection.
- Loss or fracture of a temporary or permanent crown/filling.
Key Takeaways
- Root canal therapy can save your natural teeth and relieve pain.
- The procedure is commonly performed, safe, and typically no more uncomfortable than a regular filling.
- Following aftercare instructions and completing permanent restoration is crucial for long-term success.
- Regular dental hygiene and checkups reduce the risk of future dental infections.
Read full bio of medha deb












