Understanding Venous Disease: Causes, Symptoms, and Modern Treatments
Explore venous disease causes, symptoms, risk factors, and the latest effective treatments for improved vein health and quality of life.
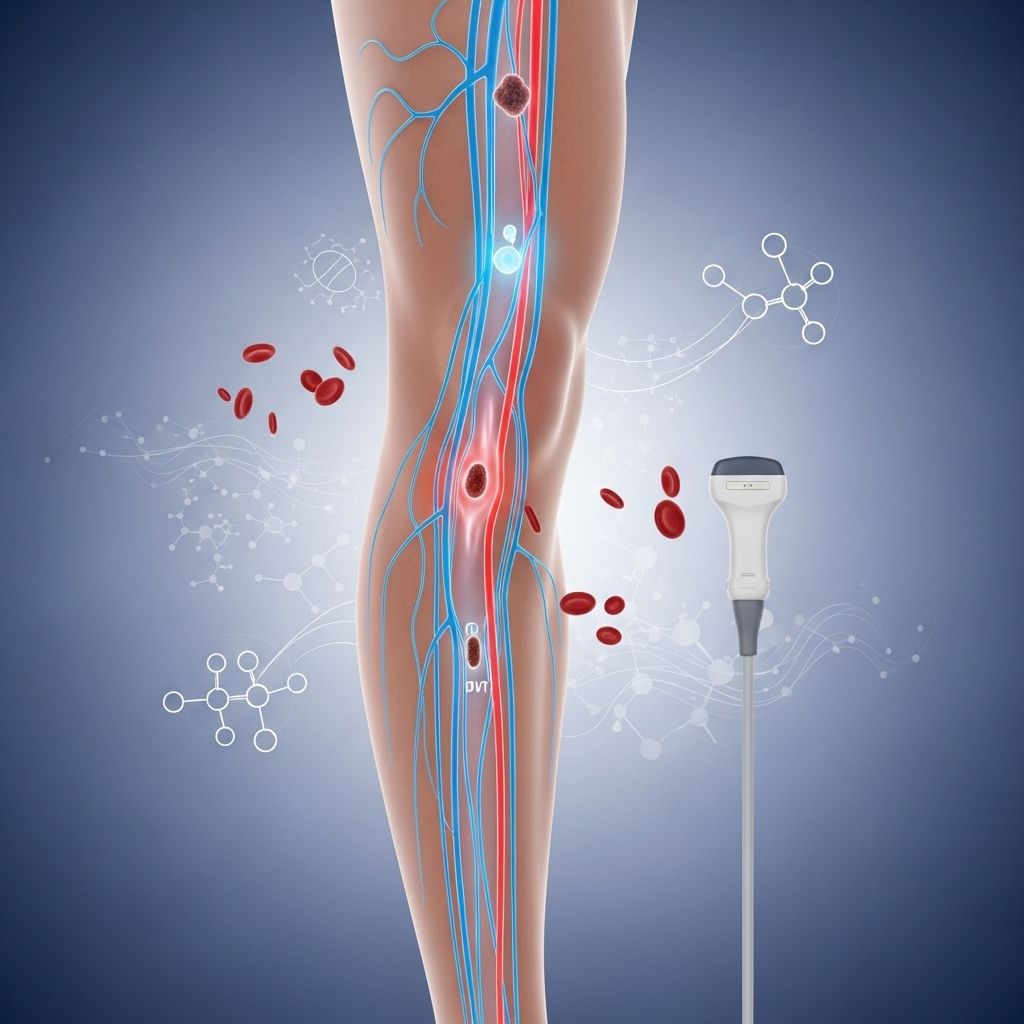
What Is Venous Disease?
Venous disease refers to a range of conditions affecting veins, most commonly in the legs, caused by improper functioning of the vein valves necessary for returning blood to the heart. When these valves become faulty or damaged, blood flow is hindered, often resulting in blood pooling in the lower limbs and a variety of symptoms and complications that can impact quality of life.
Types of Venous Disease
- Chronic Venous Insufficiency (CVI): A persistent condition where weakened or damaged vein valves cause blood to flow backwards and pool in the legs, also known as venous reflux.
- Varicose Veins: Enlarged, twisted, and visible veins often resulting from chronic venous insufficiency.
- Spider Veins: Small, superficial veins that appear as thin lines, webs, or branches, typically considered a milder form of venous disease.
- Deep Vein Thrombosis (DVT): A serious condition where blood clots form in deep veins, usually in the legs. DVT can be both a cause and a result of venous insufficiency.
- Leg Ulcers: Open sores or wounds on the legs, commonly developing from longstanding venous insufficiency.
- Peripheral Venous Disease (PVD): Encompasses a spectrum of disorders involving vein malfunction and poor circulation in the limbs, often linked to the above conditions.
How Veins Function and What Goes Wrong
In healthy veins, one-way valves ensure that blood travels upward toward the heart against gravity. When these valves fail or become weakened, blood leaks backward and accumulates in the lower limbs, resulting in increased venous pressure and the characteristic symptoms of venous disease. This backward flow is known as venous reflux and is the hallmark of chronic venous insufficiency (CVI).
Difference Between Arteries and Veins
| Feature | Arteries | Veins |
|---|---|---|
| Direction of Blood Flow | Away from heart | Toward heart |
| Oxygenation | Oxygen-rich (except pulmonary) | Oxygen-poor (except pulmonary) |
| Valves Present? | No | Yes |
| Common Disorders | Atherosclerosis | Venous insufficiency, varicose veins |
Signs and Symptoms of Venous Disease
- Varicose veins: Twisted, enlarged, and visible veins under the skin, often blue or purple.
- Spider veins: Web-like clusters of thin, red, purple or blue veins visible on the skin surface.
- Leg swelling: Edema, especially around the ankles and lower legs, which may worsen after standing or sitting for long periods.
- Aching, heaviness, or fatigue in the legs: Often described as throbbing or cramping, and may be worse at the end of the day.
- Skin changes around the ankles: Discoloration (brownish or reddish), thickening, or dryness (stasis dermatitis).
- Venous ulcers: Open sores or wounds that heal slowly or recur, usually near the ankles.
- Itching, burning, or tingling: Sensations in the affected limbs.
- Leg cramps: Especially at night or after long periods of inactivity.
- Blood clots (DVT): May cause redness, warmth, pain, and swelling in a limb. This is a medical emergency.
If you experience any of these symptoms, especially persistent swelling, discoloration, or ulcers, consult a healthcare professional for assessment and diagnosis.
Causes and Risk Factors of Venous Disease
- Faulty or weakened vein valves: These are the primary contributors to chronic venous insufficiency and varicose veins, allowing blood to flow backward.
- Genetics/family history: Venous disease often runs in families.
- Age: Risk increases with age, especially over 50.
- Gender: Women are more likely to develop venous disease, partly due to hormonal factors and pregnancy.
- Prolonged standing or sitting: Occupations or lifestyles requiring extended immobility can increase risk due to sustained pressure in the leg veins.
- Obesity: Excess weight increases pressure on lower limb veins.
- Pregnancy: Hormonal changes and increased blood volume during pregnancy can stretch vein walls and encourage valve dysfunction.
- Prior leg injuries or blood clots (DVT): These can damage vein valves or walls, increasing the risk of future venous problems.
- Inactivity and sedentary lifestyle: Lack of movement decreases calf muscle contraction, which normally assists blood return from the legs.
- Other medical conditions: Such as congestive heart failure or peripheral artery disease (PAD), which can complicate venous disease and its management.
Addressing modifiable risk factors, such as weight, physical activity, and posture, plays an important role in prevention and treatment.
Diagnosing Venous Disease
Timely and accurate diagnosis is essential for effective management and prevention of complications. The diagnostic process includes:
- Medical history and physical examination: Assessment of symptoms, lifestyle, and risk factors, along with a thorough examination of the legs for visible signs (swelling, discoloration, ulcers, or varicose veins).
- Doppler ultrasound: A noninvasive imaging technique that visualizes blood flow in the veins, evaluates valve function, and detects clots or blockages.
- Duplex ultrasonography: Combines traditional ultrasound and Doppler to provide a detailed assessment.
- Other tests: In certain cases, MRI or CT scans may be used to rule out underlying causes or other vascular conditions (such as peripheral artery disease).
Your healthcare provider may also evaluate for concomitant peripheral artery disease (PAD) and tailor your treatment plan accordingly, as PAD can affect treatment choices (especially compression therapy).
Treatment Options for Venous Disease
Treatment aims to relieve symptoms, prevent complications, and improve vein function. The recommended approach depends on the severity, type, and cause of venous disease, as well as the patient’s overall health.
Conservative and Lifestyle Approaches
- Compression stockings or bandages: Medical-grade compression garments help support veins, reduce swelling, and improve blood flow. These are a first-line therapy and can be prescribed in various strengths.
- Leg elevation: Periodically raising the legs, especially above heart level, helps counteract gravity, reduce swelling, and improve comfort.
- Exercise: Activities like walking and calf raises boost calf muscle pump action, which aids blood return and helps prevent stagnation.
- Weight management: Maintaining a healthy weight reduces strain on the venous system.
- Dietary changes: Reducing salt intake can help minimize swelling. Increasing fiber and nutrient-rich foods may promote vein health.
- Quitting smoking: Smoking is a risk factor for blood vessel damage and thrombosis.
- Avoiding long periods of inactivity: Taking breaks to stand, stretch, or move promotes healthy circulation.
Medication
- Blood-thinning medications (anticoagulants): Prescribed if there is a risk of blood clots or deep vein thrombosis (DVT).
- Other medications: Diuretics (to reduce swelling) or drugs that improve vein wall tone in select cases.
Minimally Invasive Procedures
- Endovenous laser treatment (EVLT): A catheter-delivered laser heats and closes the problematic vein.
- Radiofrequency ablation: Similar to laser, but uses radio waves to shut the vein.
- Sclerotherapy: A solution is injected into varicose or spider veins, causing them to collapse and disappear over time.
- Microphlebectomy: Small incisions are made to remove surface varicose veins; this is performed under local anesthesia in an outpatient setting.
- Catheter-based interventions: For deep vein issues, a catheter may be used to deliver treatment directly to the vein (recanalization, ballooning, and stenting).
- IVC (Vena cava) filter placement: In rare cases, filters may be inserted to prevent blood clots from traveling to the lungs.
Surgical Options
- Surgical vein stripping or ligation: In select advanced cases, abnormal veins are removed or tied off to reroute blood flow through healthier vessels.
Most treatments are highly effective and can greatly improve symptoms, appearance, and quality of life. Your provider will recommend the best fit for your circumstances based on exam findings and diagnostic results.
Complications and Prevention
- Leg ulcers: Result from severe, longstanding venous insufficiency and are prone to infection.
- Blood clots (DVT): Can be life-threatening if they move to the lungs (pulmonary embolism).
- Chronic pain and discomfort: May decrease mobility and quality of life.
Preventive strategies include:
- Maintaining physical activity and healthy weight
- Wearing compression stockings as recommended
- Elevating the legs when possible
- Avoiding prolonged immobilization
- Managing existing health conditions (such as heart failure or high blood pressure)
- Promptly addressing early symptoms with medical consultation
Frequently Asked Questions (FAQs) About Venous Disease
Q: Is venous disease only cosmetic?
A: No. While spider and varicose veins may appear to be a cosmetic concern, venous disease can be progressive and may cause pain, swelling, ulcers, and other complications if not addressed.
Q: Can men develop venous disease?
A: Yes. Although more common in women, especially during and after pregnancy, men can also develop venous insufficiency and associated conditions. Age, hereditary factors, inactivity, and obesity all play a role.
Q: Are minimally invasive treatments safe?
A: Most minimally invasive treatments for venous disease, such as endovenous ablation and sclerotherapy, are considered safe and effective, with short recovery times and minimal complications when performed by specialists.
Q: Can I prevent venous disease if it runs in my family?
A: While you cannot change hereditary risk, leading a healthy lifestyle (weight management, regular exercise, not smoking), wearing compression garments if prescribed, and early management of symptoms can reduce your risk and slow progression.
Q: When should I see a vein specialist?
A: You should seek medical advice if you develop persistent swelling, pain, skin color changes, non-healing sores, or notice significant changes in the appearance of your veins, especially if symptoms interfere with daily life or mobility.
When to See a Physician
- Persistent leg swelling, especially if sudden in onset
- Pain, tenderness, redness, or warmth in a leg (potential blood clot — seek immediate attention)
- Development of ulcers, wounds, or significant skin changes near the ankles
- Varicose veins that cause aching, cramping, or interfere with daily activities
Prompt evaluation by a vein specialist or vascular medicine physician ensures accurate diagnosis and access to effective modern therapies. Early management prevents complications such as painful ulcers or blood clots. Most people can achieve symptom relief and improved function with proper care.
Read full bio of medha deb












