Wisdom Tooth Removal: Complete Guide to the Procedure
Everything you need to know about wisdom tooth extraction, from reasons for removal to recovery and aftercare
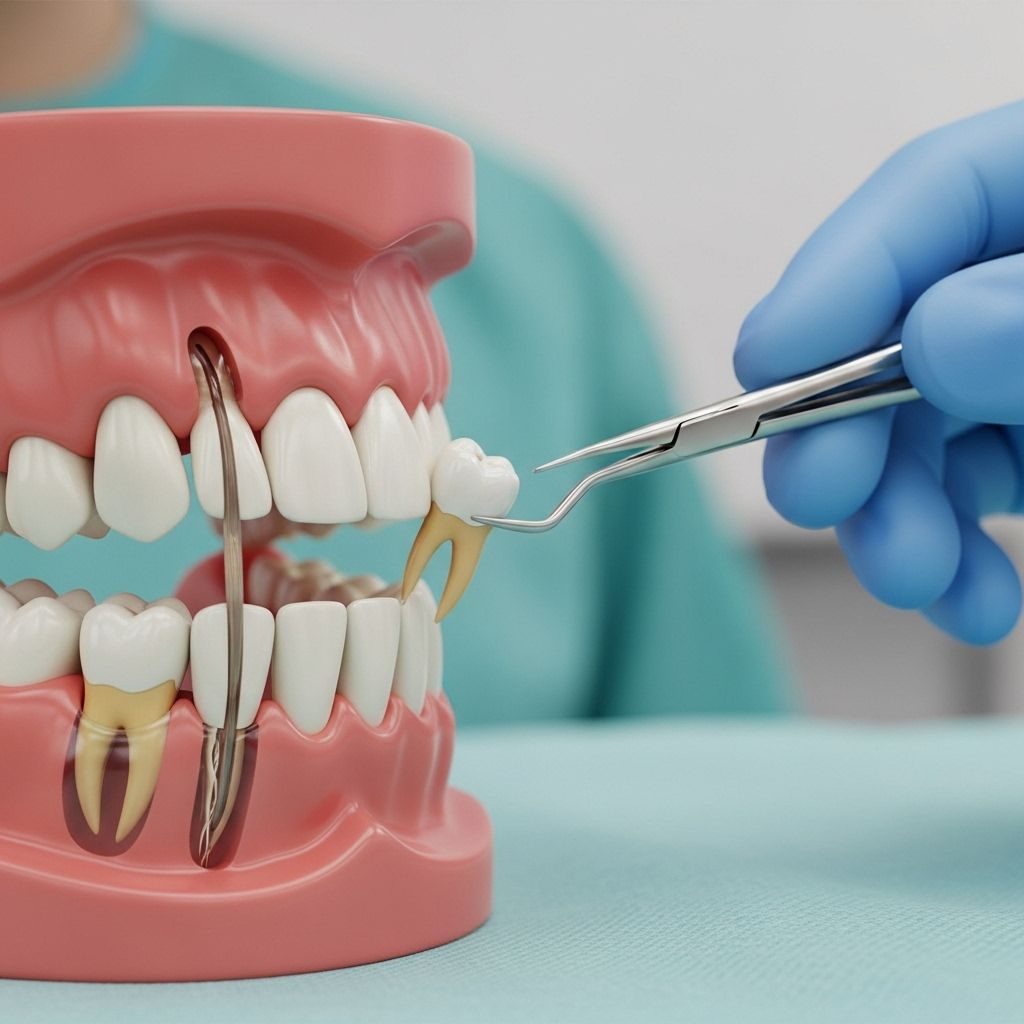
Wisdom teeth, also known as third molars, are the last teeth to develop in your mouth. They typically emerge during the late teenage years or early twenties, though complications can arise at any age. When these teeth don’t have sufficient space to grow properly or become impacted, removal may be necessary to prevent various dental problems. Understanding the wisdom tooth removal process, from initial consultation to full recovery, can help alleviate concerns and prepare you for what to expect.
Understanding Why Wisdom Teeth Need Removal
Wisdom teeth develop much later than other teeth, usually making their appearance during adolescence or early adulthood. While some people’s wisdom teeth emerge without any issues, many individuals experience complications that necessitate removal. The primary reason for extraction is insufficient space in the mouth for these teeth to come through properly.
When wisdom teeth lack adequate room to develop, they may become impacted, meaning they’re blocked by another tooth or only partially break through the gum line. This problematic positioning can lead to numerous dental health issues that affect both comfort and oral hygiene. Your dentist will typically use X-rays to assess the positioning of your wisdom teeth and determine whether removal is necessary.
Several complications can arise from impacted or poorly positioned wisdom teeth. Pain and swelling are among the most common symptoms, often indicating that the tooth is pressing against adjacent teeth or struggling to emerge through the gum tissue. This discomfort can range from mild to severe and may come and go in waves as the tooth attempts to break through.
Pericoronitis, an infection of the gum tissue surrounding a partially erupted wisdom tooth, represents another frequent complication. This condition occurs when bacteria become trapped beneath the gum flap covering the tooth, leading to inflammation, pain, and sometimes fever. Food particles and bacteria can easily become lodged in the space between the gum and the partially emerged tooth, creating an ideal environment for infection.
The positioning of wisdom teeth makes them particularly difficult to clean properly, which increases the risk of tooth decay and gum disease. Even when wisdom teeth do emerge fully, their location at the back of the mouth makes thorough brushing and flossing challenging. This difficulty in maintaining proper oral hygiene can lead to cavities not only in the wisdom teeth themselves but also in the adjacent molars.
More serious complications include the formation of cysts, which are fluid-filled sacs that develop around the tooth. These cysts can damage the surrounding bone and teeth if left untreated. Additionally, dental abscesses may form when bacterial infection spreads to the tooth pulp or surrounding tissues, causing severe pain and potentially systemic health issues if the infection enters the bloodstream.
It’s important to note that not all wisdom teeth require removal. If your wisdom teeth have emerged properly, are positioned correctly, and aren’t causing any problems, your dentist will typically recommend monitoring them during routine dental check-ups rather than extracting them. Regular monitoring allows your dental professional to catch any developing issues early before they become more serious.
The Wisdom Tooth Removal Procedure Explained
The process of removing wisdom teeth can vary significantly depending on the tooth’s position, development stage, and complexity of extraction. A general dentist may perform straightforward extractions in their office, but more complicated cases often require referral to an oral surgeon or specialist at a hospital, clinic, or specialized dental surgery facility.
Before the extraction begins, your dental professional will discuss anaesthetic options with you. The choice of anaesthesia depends on several factors, including the difficulty of the extraction, the number of teeth being removed, your medical history, and your anxiety level about the procedure.
Anaesthetic Options
Local anaesthetic is the most commonly used option for wisdom tooth removal. This involves an injection into the gum tissue surrounding the tooth, similar to what you might receive for a dental filling. The anaesthetic takes just a couple of minutes to numb the area completely, ensuring you won’t feel pain during the extraction. You’ll remain fully conscious and aware during the procedure, though you may feel pressure and hear sounds as the dentist works. The numbness typically extends to your lower lip and tongue and can last for several hours after the procedure. If you’re having local anaesthetic only, you should eat normally before your appointment.
Intravenous sedation may be offered in addition to local anaesthetic for more difficult extractions or for patients who experience dental anxiety. This sedation is administered through a vein in your arm and makes you feel drowsy and relaxed while remaining conscious enough to respond to instructions. Many patients remember little of the procedure afterward. This option provides a middle ground between being fully awake and completely asleep.
General anaesthetic puts you completely to sleep during the procedure and is typically reserved for particularly difficult extractions or when multiple wisdom teeth are being removed simultaneously. Most wisdom tooth removals under general anaesthetic are performed as day-case procedures, meaning you’ll go home the same day. However, you’ll need to attend a pre-assessment appointment beforehand to ensure you’re fit for the procedure. On the day of surgery, you must arrange for someone to collect you and stay with you for at least 24 hours afterward. Following general anaesthetic, it’s recommended to take up to a week off work for recovery.
Steps of the Extraction
Once the anaesthetic has taken effect, the dentist or surgeon will begin the extraction process. If the wisdom tooth hasn’t fully emerged through the gum, the first step involves making a small incision in the gum tissue to access the tooth. In some cases, a small amount of bone covering the tooth may also need to be removed to facilitate extraction.
The dentist will then work to widen the tooth socket by gently rocking the tooth back and forth. You’ll likely feel pressure during this stage, which is completely normal and doesn’t indicate that the anaesthetic isn’t working. If you do experience pain at any point during the procedure, it’s crucial to inform your dentist or surgeon immediately so they can administer additional anaesthetic.
For teeth that are more difficult to remove, the dentist may need to cut the tooth into two or three smaller pieces. This technique makes it easier to remove the tooth through the opening in the gum without having to remove excessive amounts of bone. Once the tooth or tooth fragments have been completely removed, the dentist will clean the extraction site thoroughly.
If an incision was made in the gum, the dentist will place stitches to close the wound. In the majority of cases, these stitches are dissolvable and will fall out on their own within 10 to 21 days, eliminating the need for a follow-up appointment to have them removed. After the extraction is complete, the surgeon will place gauze over the extraction site and ask you to bite down firmly for up to an hour. This pressure helps form a blood clot in the empty tooth socket, which is an essential part of the healing process.
Duration and Recovery Timeline
The time required to remove a wisdom tooth varies considerably depending on its position and the complexity of the extraction. Simple, straightforward extractions where the tooth has fully emerged and can be removed in one piece may take only a few minutes. More complicated cases involving impacted teeth, bone removal, or cutting the tooth into sections can take 20 to 40 minutes per tooth.
Most wisdom tooth removal procedures are completed within 45 minutes, though this can extend longer if multiple teeth are being extracted during the same appointment. Your dental professional will provide you with a more accurate time estimate based on your specific situation after reviewing your X-rays and examining your teeth.
Following the extraction, you’ll typically go home the same day, even if you had a general anaesthetic, provided you’re suitable for day-case treatment. If complications arise or if you had a particularly complex extraction, you might need to stay in the hospital overnight for observation.
What to Expect After Wisdom Tooth Removal
Recovery from wisdom tooth extraction is a gradual process that varies from person to person. Understanding what’s normal during the healing period can help you manage expectations and recognize when something might require attention from your dentist.
Immediate Post-Operative Symptoms
Discomfort and pain are expected after wisdom tooth removal. The intensity typically peaks during the first three days following surgery but should gradually decrease over the next two weeks. Most patients require regular pain relief medication for three to four days after the procedure. Over-the-counter options like paracetamol or ibuprofen, taken according to package directions, are usually sufficient to manage the discomfort. If you’ve been prescribed stronger pain medication, follow your dentist’s instructions carefully and avoid taking additional over-the-counter painkillers without checking for potential interactions.
Swelling and bruising commonly occur after wisdom tooth extraction. The swelling usually reaches its peak one to two days after the operation and may affect both the inside and outside of your mouth. External swelling on your face or jaw is normal and shouldn’t cause alarm. The swelling should begin to subside after the first few days, though it may take up to two weeks to disappear completely. Bruising may also develop on the skin of your face, appearing as discoloration that can take up to a fortnight to fade completely.
Jaw stiffness and restricted mouth opening are normal consequences of wisdom tooth surgery. The muscles and tissues around the extraction site may feel tight, making it difficult to open your mouth as wide as usual. This limitation can make eating challenging, and you’ll likely need to stick to a soft food diet for approximately one week. The stiffness should gradually improve over seven to ten days as the tissues heal.
Minor bleeding is common for the first day or two after surgery. Some oozing of blood mixed with saliva is normal and should decrease progressively. If bleeding becomes heavy or persistent, bite down on a clean gauze pad placed directly over the extraction site for 30 minutes. Avoid repeatedly spitting, as this can dislodge the blood clot and prolong bleeding.
Managing Your Recovery
Proper aftercare significantly influences how quickly and smoothly you recover from wisdom tooth removal. Your dentist will provide specific post-operative instructions, but general guidelines include avoiding vigorous rinsing for the first 24 hours, as this can disturb the blood clot. After the first day, gentle rinsing with warm salt water can help keep the area clean and promote healing.
Avoiding smoking, drinking through straws, and consuming alcohol during the initial healing period is crucial, as these activities can dislodge the blood clot and lead to a painful condition called dry socket. Maintaining good oral hygiene by carefully brushing around the extraction site without disturbing it directly helps prevent infection while allowing the area to heal.
In some cases, your dentist may prescribe antibiotics to prevent or treat infection, particularly if there was an ongoing infection before the extraction or if the procedure was particularly complex. Take the full course of antibiotics as directed, even if you start feeling better before finishing the medication.
Potential Risks and Complications
While wisdom tooth removal is a common and generally safe procedure, as with any surgical intervention, certain risks and potential complications exist. Being aware of these possibilities helps you recognize warning signs that may require additional medical attention.
The most common risks include pain, bleeding, bruising, swelling, and infection, all of which have been discussed in detail above. Most of these complications are mild and resolve with proper care and time. However, occasionally more serious issues can develop.
Dry socket occurs when the blood clot in the tooth socket becomes dislodged or fails to form properly, exposing the underlying bone. This condition typically develops three to four days after extraction and causes severe, throbbing pain that may radiate to the ear. Dry socket requires treatment from your dentist, who will clean the socket and place a medicated dressing to promote healing and relieve pain.
Nerve damage is a rare but potential complication, particularly with lower wisdom teeth. The nerves supplying sensation to the lower lip, chin, and tongue run close to the roots of lower wisdom teeth. In some cases, these nerves can be bruised or damaged during extraction, resulting in temporary or, very rarely, permanent numbness or altered sensation in these areas. Your dentist will discuss this risk with you if your X-rays show that your tooth roots are close to these nerves.
Sinus complications can occur when upper wisdom teeth are removed, as their roots sometimes extend into the sinus cavity. Removal may create a small opening between the mouth and sinus, though this usually heals on its own. Rarely, further treatment may be needed to close the opening.
Contact your dentist if you experience excessive bleeding that doesn’t stop with pressure, severe pain that isn’t controlled by prescribed medication, signs of infection such as fever, increasing swelling after the first few days, difficulty breathing or swallowing, or numbness that persists beyond the expected duration of local anaesthetic.
Making the Decision About Wisdom Tooth Removal
Not everyone needs to have their wisdom teeth removed. The decision should be based on a thorough examination, X-ray evaluation, and discussion of symptoms and risks with your dentist. If your wisdom teeth have emerged properly, are positioned correctly, can be cleaned adequately, and aren’t causing any problems, your dentist will likely recommend a watch-and-wait approach with regular monitoring during routine dental check-ups.
However, if problems develop or X-rays show that issues are likely to occur, removal is often the best course of action. Younger patients typically experience easier extractions and faster recovery times, as the tooth roots are not fully formed and the surrounding bone is less dense. This is why dentists sometimes recommend removing potentially problematic wisdom teeth in late adolescence or early twenties, even before symptoms develop.
Your dentist will consider multiple factors when recommending wisdom tooth removal, including the position and angle of the teeth, the amount of space available in your jaw, your oral hygiene ability, your history of problems with wisdom teeth, and your overall dental health. They’ll work with you to create a treatment plan that addresses your specific situation while minimizing risks and discomfort.
Frequently Asked Questions
Q: Will I feel pain during the wisdom tooth removal procedure?
A: No, you should not feel pain during the procedure because the area will be completely numb from the local anaesthetic. You may feel pressure and hear sounds, but these sensations are normal. If you do experience pain, inform your dentist immediately so they can provide additional anaesthetic.
Q: How long does it take to fully recover from wisdom tooth removal?
A: Initial discomfort typically lasts three to four days, with most pain subsiding within a week. Complete healing of the extraction site takes several weeks to months, though you should be able to return to normal activities within a few days to a week, depending on whether you had local or general anaesthetic.
Q: Can I eat normally after having my wisdom teeth removed?
A: You’ll need to follow a soft food diet for approximately one week after extraction. Start with cold, soft foods like yogurt, ice cream, and smoothies, gradually progressing to warmer soft foods as healing progresses. Avoid hard, crunchy, or chewy foods that could disturb the extraction site or become lodged in the socket.
Q: What should I do if my stitches come out early?
A: Dissolvable stitches typically fall out between 10 and 21 days after surgery. If they come out slightly earlier but you’re not experiencing bleeding or other problems, this is usually fine. However, if stitches come out within the first few days and you have bleeding or the wound appears open, contact your dentist for advice.
Q: How do I know if I have an infection after wisdom tooth removal?
A: Signs of infection include increasing pain and swelling after the first few days, fever, persistent bad taste or smell in your mouth, pus discharge from the extraction site, or difficulty swallowing. If you experience any of these symptoms, contact your dentist promptly for evaluation and possible antibiotic treatment.
Q: Is it better to have all wisdom teeth removed at once or separately?
A: This depends on your individual situation. Having multiple wisdom teeth removed at once means one recovery period rather than several, which many patients prefer. However, the recovery may be more intense. Your dentist will recommend the best approach based on the complexity of your extractions, your general health, and your personal preferences.
Q: Will I need time off work or school after wisdom tooth removal?
A: This depends on the type of anaesthetic used and the complexity of the extraction. If you have local anaesthetic only, you may be able to return to work or school the next day. Following general anaesthetic, up to a week off is recommended. Your dentist can provide a more specific recommendation based on your procedure and occupation.
Read full bio of Sneha Tete












